In Vitro Fertilization
The NYU Langone Fertility Center has a world-renowned in vitro fertilization (IVF) program known for its high pregnancy success rates. IVF is the most efficient way for couples to achieve pregnancy when they are experiencing trouble conceiving.
In order for pregnancy to naturally occur, sperm must travel through the uterus to one of the fallopian tubes, where it fertilizes an egg. The resulting embryo must be of good quality in order for implantation to occur.
While the process sounds simple, there are multiple factors that can stop these steps from happening, such as a low sperm count, a compromised or blocked fallopian tube, a damaged or diseased uterus, or suboptimal egg production or quality. When the sperm and egg are unable to meet on their own, or egg or sperm quality is lower than desired, IVF may be an option.
During IVF, eggs are retrieved from the ovaries—or donor eggs may be used—and fertilized with sperm acquired either from a partner or a donor. The resulting embryo is inserted into the uterus, where it ideally implants and creates a pregnancy.
People having IVF must attend an orientation session conducted by our staff before beginning treatment. Partners are encouraged to attend this session as well. In addition to attending a scheduled session, you can also view our orientation.
While every woman’s cycle is unique, here is a general overview of the IVF process.
Step One: Ovulation Induction
During a typical menstrual cycle, the ovaries release one egg each month. In preparation for IVF, fertility drugs, called gonadotropins, are self-administered daily to stimulate the ovaries to mature numerous eggs in the month of the treatment cycle. If more eggs are matured, more can be harvested and used. Most often, this improves the chances of fertilization and, ultimately, pregnancy.
Step Two: Egg Retrieval (Oocyte Retrieval)
When the eggs, also known as oocytes, are ready to be retrieved from the body, a procedure is performed at the Fertility Center using mild sedation. The doctor—with the aid of ultrasound visualization—guides a needle through the vagina wall and into the ovaries. An anesthesiologist is present for all procedures.
After the eggs are retrieved, they are fertilized with sperm in the embryology laboratory. Success rates vary depending on a person’s age, response to the medication, and the quality of the eggs and embryos produced.
As with all surgical procedures, there are risks associated with egg retrieval that should be discussed with your doctor.
Step Three: Fertilization in the Lab
When the eggs arrive in the embryology lab, our staff analyzes them for maturity and then places the eggs into an incubator that has an environment similar to the one inside the body. In most cases, sperm is combined with the eggs and fertilization occurs naturally. In situations where low sperm count or low sperm motility (movement) is a factor, a single sperm is injected directly into each mature egg in a process called intracytoplasmic sperm injection (ICSI).
Once the egg and sperm are combined, it takes approximately 18 hours to determine whether fertilization has occurred and another 2 to 4 days to establish whether the embryo is optimally developing. The embryos most often stay in the laboratory for a total of five days.
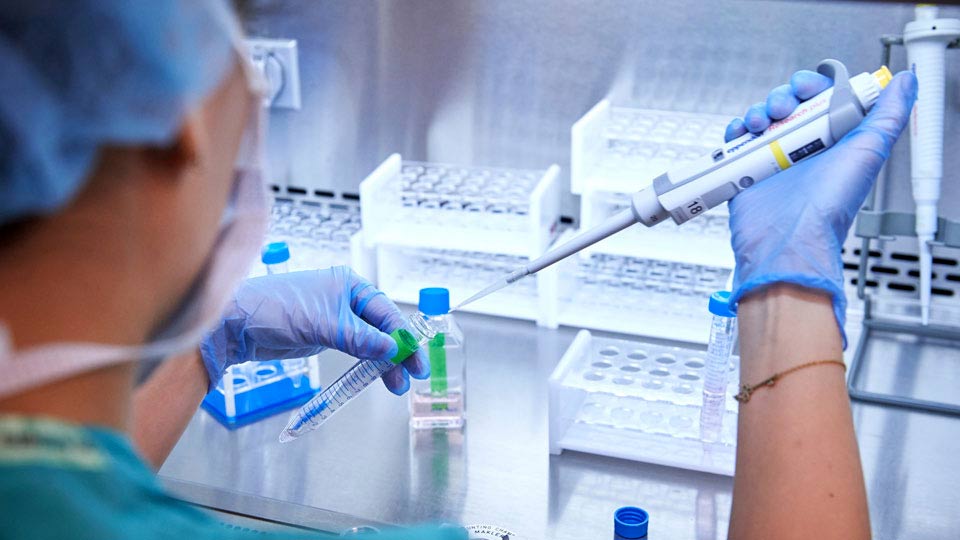
In 80 percent of our current patient cycles, preimplantation genetic screening (PGS) of the created embryos is performed at this stage to assess the chromosomal integrity of the created embryos.
Step Four: Embryo Transfer
In preparation for the embryo transfer, the doctor discusses the number of embryos produced as well as the quality of each. Grading is a tool physicians and embryologists use to determine which embryos to transfer and when. One of the Fertility Center’s goals is to limit the number of embryos transferred in order to limit the number of multiple births. In more than 60 percent of the embryo transfers we perform, only a single embryo is placed into the uterus.
Embryo transfer is a simple technique, and anesthesia or sedation is rarely required. A long, thin catheter containing the agreed upon number of embryos, along with a small amount of fluid, is passed through the cervix into the uterus, where the embryo or embryos are released. An abdominal ultrasound is simultaneously performed to ensure optimal placement in the uterus.
Following the embryo transfer, limitation of rigorous physical activity is recommended for several days.
After an Embryo Transfer
After a blastocyst embryo transfer is completed, it takes about nine days before a pregnancy can be detected. During the days after a transfer, the following happens to the embryo:
- Day 1: The blastocyst begins to hatch out of its shell.
- Day 2: The blastocyst continues to hatch out of its shell and begins to attach itself to the uterus.
- Day 3: The blastocyst attaches deeper into the uterine lining, beginning implantation.
- Day 4: Implantation continues.
- Day 5: Implantation is complete. Cells that eventually become the placenta and fetus have begun to develop.
- Day 6: Human chorionic gonadotropin (hCG), the hormone that signals a developing pregnancy, starts to enter the blood stream.
- Days 7 and 8: Fetal development continues and hCG continues to be secreted.
- Day 9: Levels of hCG are now high enough in maternal blood to detect a pregnancy using a blood test.
Embryo Freezing or Cryopreservation
Embryos are cryopreserved, or frozen, for multiple reasons. The traditional IVF process often results in more embryos than can be transferred into the uterus in one cycle. If the non-transferred embryos are of acceptable quality, they can be frozen and stored for future use. Embryos are also frozen after preimplantation genetic screening has been performed. In addition, embryo freezing is a way for people to delay childrearing until a more appropriate time in their lives.
Cryopreservation of embryos reduces the need for repeated ovarian stimulation. Instead of IVF, future cycles can be embryo transfers, which are less difficult, both physically and financially.
Complex Types of IVF
At the Fertility Center, we consider IVF to be “complex” if prior attempts have been unsuccessful, if sperm counts or motility are severely low, or if the quality of the resulting embryos has been poor. This last reason may be due to many factors; most commonly it’s related to advanced maternal age, but it may also be due to endocrine disorders, such as polycystic ovary syndrome. When very severe male infertility requires surgical extraction of sperm, this is also considered to be a complex type of IVF.
Contact Us
To schedule an appointment, contact one of our specialists or call the Fertility Center at 212-263-8990.