Surgery for Meningioma
For people with meningiomas that are causing symptoms or are growing, and for those with atypical or cancerous tumors, NYU Langone doctors usually recommend surgery.
Surgical Planning and Preparation
Surgical planning is based on a neurological examination and a study of the MRI and CT scans. Depending on its location, the tumor may involve important blood vessels. If so, an angiogram may be needed to see how the tumor is affecting these vessels and also to identify vessels that might be supplying blood to the tumor.
An angiogram is a type of X-ray that creates images of the blood vessels that supply oxygen and other nutrients to the meningioma, helping it to grow. Before the test, a contrast dye is injected through a catheter into the arteries that lead to the brain to create more detailed images of the tumor and surrounding blood vessels.
In certain situations, doctors may inject a substance that blocks the blood supply to the tumor. This procedure, called embolization, is performed at the time of the angiogram to reduce the amount of bleeding during surgery. Surgeons called interventional neuroradiologists perform these procedures.
An angiogram is rarely needed for a meningioma of the spinal cord because such tumors don’t usually involve critical blood vessels.
Surgical Guidance and Monitoring
Image guidance may be used to pinpoint the location of a tumor under the skull. This allows the surgeon to create an opening in the skull just large enough and precisely located over the tumor, thus avoiding exposure of other parts of the brain.
Image guidance is provided by a computer used during surgery that incorporates MRI and CT scans. This approach can also be used to remove meningiomas of the spinal cord. Our neurosurgeons also use ultrasound to locate the spinal cord tumors and guide the procedure.
During surgery involving the brain and spinal cord, surgeons receive real-time information about a person’s neurological function, which helps them minimize inadvertent injury to nearby nerves, the brain, or the spinal cord. Neurophysiologists, the doctors who provide this special monitoring, are present in the operating room during the entire surgery.
Types of Surgery
The type of surgery performed depends on the size and location of the meningioma.
Craniotomy
Surgeons may perform a craniotomy, a procedure to open the skull, for a meningioma found on the brain’s surface. Craniotomy may also be used for tumors found in some areas of the skull base, such as near the brainstem, where the brain meets the spinal cord.
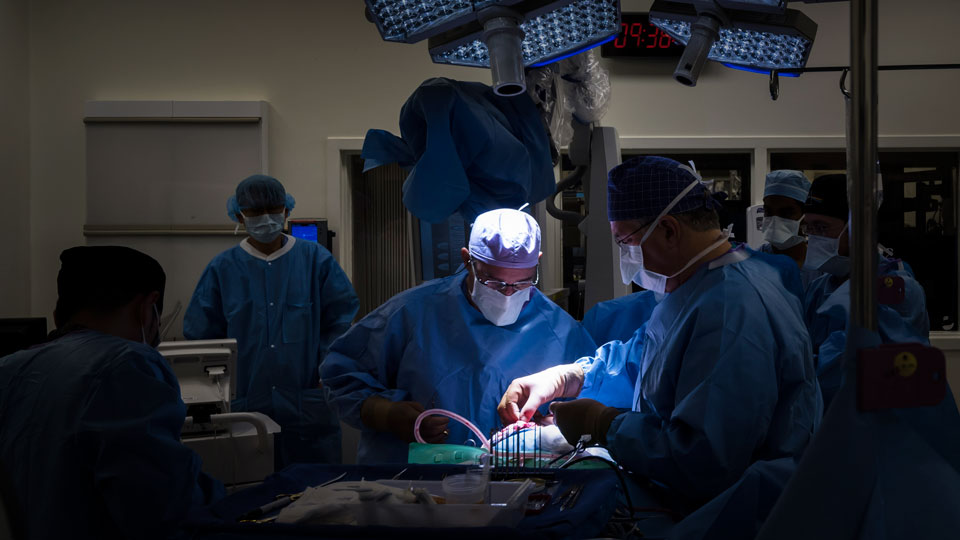
A craniotomy is performed using general anesthesia. A surgeon makes an incision in the scalp and removes a small part of the skull to create an opening. A surgical microscope is often used to provide a high magnification of the tumor and surrounding critical structures. Using microinstruments—very small tools used to perform complex surgeries—the surgeon removes as much of the growth as possible.
Afterward, the doctor closes the hole with the removed portion of skull and stitches the skin together.
Endoscopic Endonasal Surgery
For a meningioma in the skull base that can be reached through the nose, a doctor may perform endoscopic endonasal surgery. This approach requires general anesthesia but is minimally invasive, meaning it doesn’t require opening the skull. Neurosurgeons, who specialize in brain surgery, and surgical otolaryngologists, doctors who specialize in ear, nose, and throat surgery, work as a team to perform the procedure.
This approach involves the use of an endoscope, a long, thin, lighted tube with a tiny camera on it, which enables the surgical team to see inside the body. The surgeon places the endoscope through the nose and sinuses—the air-filled cavities on either side of the nose—and into the skull base.
Doctors view the tumor and the complex skull base structures, including important nerves and blood vessels, through the endoscope. Using tiny surgical tools placed through the nose and sinuses and into the skull base, the surgical team can remove as much of the meningioma as possible.
Your neurosurgeon determines whether endoscopic endonasal surgery is an option for you.
Neuroendoscopic Surgery
In neuroendoscopic surgery, the surgeon inserts a tube through a small hole created in the skull. Through this tube, an endoscope and surgical tools are introduced under computerized image guidance, called neuronavigation, to reach tumors in the brain. This approach may be used for meningiomas found in the ventricular chambers, the inner parts of the brain that contain cerebrospinal fluid. This clear liquid cushions the brain and spinal cord.
This procedure requires general anesthesia. Because only a small opening is created, neuroendoscopic surgery is considered to be minimally invasive. The approach allows very little manipulation of the healthy brain tissue between the skull and the ventricular chambers.
After surgeons remove the meningioma, they close the small opening made in the skull and stitch or staple the incision.
Spinal Surgery
For a spinal meningioma, a surgeon makes an incision, usually in the back near the upper or middle portion of the spine, where these tumors are often found. Using microinstruments, the surgeon carefully cuts open the meninges and removes the growth, while avoiding the spinal cord and important nerves. The procedure requires general anesthesia.
Recovery After Surgery
The hospital stay after surgery for a meningioma can range from a few days to a couple of weeks, depending on how large the tumor is, where it’s located, and the type of procedure used to remove it. For example, minimally invasive procedures, such as endoscopic endonasal or neuroendoscopic surgery, may require less recovery time than a craniotomy or spinal surgery.
Throughout your recovery, our doctors ensure you are as comfortable as possible. They can prescribe medication for any discomfort, such as nausea or headache.
Our doctors also monitor brain and spinal nerve function to determine if any problems with information processing or mobility have developed as a result of surgery. These problems can be addressed with support services.
Doctors at NYU Langone’s Rusk Rehabilitation can prescribe inpatient physical and occupational therapy to people who have had surgery for a meningioma. This therapy may last for a few days to several weeks. Therapy may also be part of ongoing outpatient care. Rehabilitative programs at NYU Langone are designed to help you return to your daily activities as soon as possible.
Tissue Analysis
After surgery, an NYU Langone pathologist analyzes tumor cells under a microscope to determine whether the tumor is benign, atypical, or cancerous. This is the only way to confirm a diagnosis of meningioma. The results of this analysis guide your doctor’s recommendations about additional treatment.
If a surgeon can completely remove a tumor and confirm that it is benign, surgery may be the only treatment needed. However, doctors may prescribe radiation therapy if benign cells remain after surgery.
For a malignant or atypical meningioma, NYU Langone doctors often recommend radiation therapy after surgery.
Almost all people with a meningioma have their medical information reviewed at a multidisciplinary NYU Langone brain and spinal cord tumor conference. At this meeting, doctors, from all specialties with expertise in tumor treatment work together to make a recommendation for the best possible care.
Meet Our Doctors
Perlmutter Cancer Center specialists provide care and support during treatment.
Browse Doctors