Patients Leaving the Hospital Have Lots of Questions. NYU Grossman School of Medicine Students Help Provide the Answers.
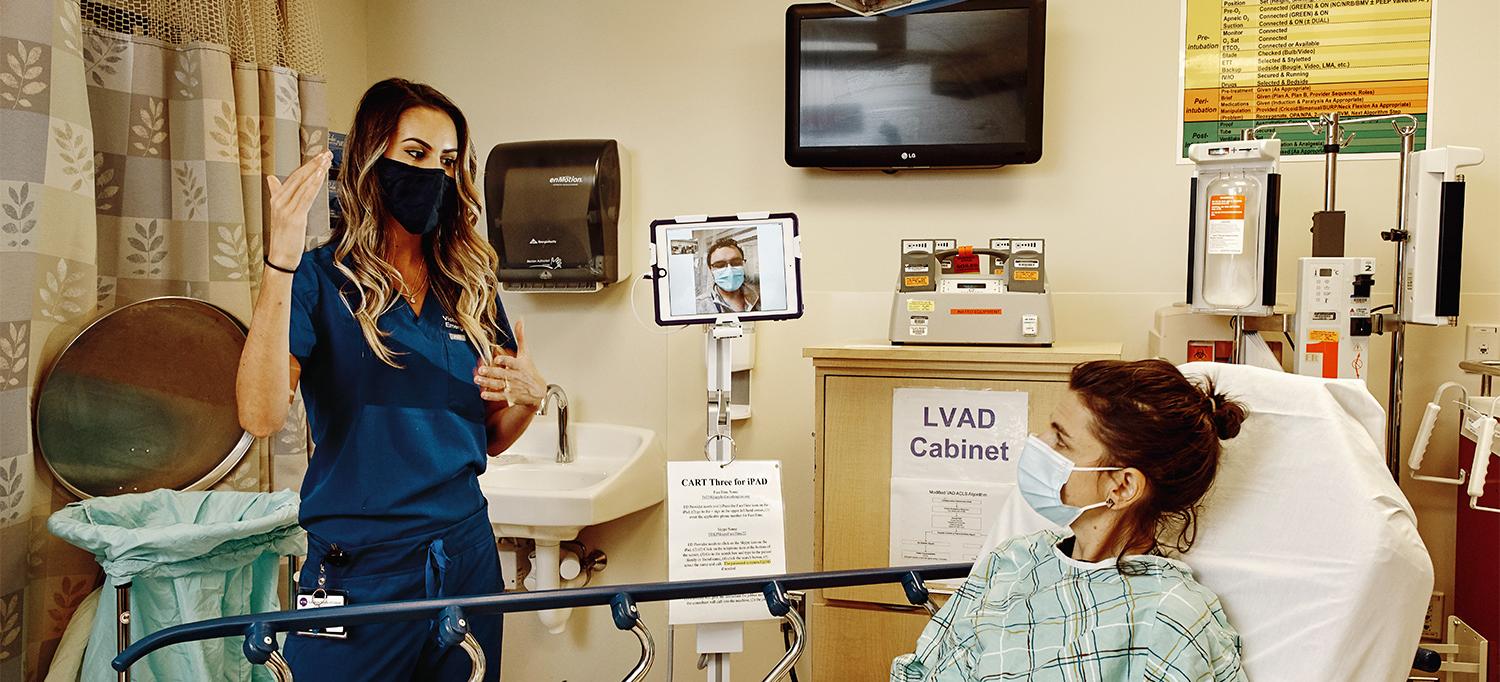
Christopher Kuhner, a fourth-year student at NYU Grossman School of Medicine—pictured on the iPad—conducts a virtual discharge counseling session with a patient as Victoria Terentiev, MD, who helped create the program, observes.
Photo: Tony Luong
During the peak of the first wave of the coronavirus disease (COVID-19) pandemic last spring, Victoria Terentiev, MD, a fourth-year resident specializing in emergency medicine at NYU Langone Hospital—Brooklyn, noticed a curious pattern: Many of the patients diagnosed with COVID-19 in the emergency department (ED) whose symptoms were mild enough to recover at home were bouncing back to the ED within a few days. In most instances, they were no sicker upon their return. Rather, they had grown increasingly anxious about their infection and how to shield the family members who live with them. The sheer volume of patients—up to 300 people visited the hospital’s ED daily, about one third more than before the surge—required clinicians to review their discharge instructions within a few minutes and move on.
“Patients with COVID-19 have lots of questions and require a longer duration of counseling,” says Dr. Terentiev. Her solution? Tap students at NYU Grossman School of Medicine, ranked No. 2 in the nation for research in U.S. News & World Report’s 2022 “Best Graduate Schools” rankings. Nancy Conroy, MD, associate chief of service for the Emergency Department at NYU Langone Hospital—Brooklyn, was intrigued by the idea of having medical students counseling patients in the ED before their discharge, but there was a logistical challenge: the students were prohibited from all clinical units. Audrey Tse, MD, clinical assistant professor for the Ronald O. Perelman Department of Emergency Medicine, came up with a workaround, suggesting that students instead consult virtually, using iPads the hospital had been given to facilitate communication between physicians and the families of hospitalized patients.
Christopher G. Caspers, MD, vice chair of clinical operations for the Ronald O. Perelman Department of Emergency Medicine, championed the project, and Ian G. Wittman, MD, chief of service for the ED at NYU Langone Hospital—Brooklyn, signed off. “It was an innovative idea with minimal risks that met everyone’s needs—patients, clinicians, and med students,” says Dr. Caspers. Linda R. Tewksbury, MD, associate dean for student affairs, meanwhile helped recruit 20 third- and fourth-year students. Dr. Terentiev and Dr. Conroy, for their part, created a 10-page script highlighting what discharged patients need to know, from the expected symptoms and recommended fever reducers, to proper hygiene practices and symptoms that might necessitate a return visit. “We used simple language patients could understand,” says Dr. Terentiev. She tutored medical students Christopher Kuhner and Joshua Ross in how to conduct video chats, access clinicians’ notes, and for the 43 percent of patients at NYU Langone Hospital—Brooklyn with COVID-19 whose primary language is one other than English, connect with a translator. In turn, Kuhner and Ross trained other students.
Since its launch last May, virtual discharge counseling has been an unqualified success. Before discharge, patients spend an average of 20 minutes speaking remotely with medical students, freeing up emergency medicine doctors and nurses to attend to other sick patients. “We knew there was a lot of uncertainty among patients, and these calm one-on-one sessions made sure they truly understood what they were being told,” says Dr. Conroy.
With all their COVID-19 questions addressed, the rate of patients returning to the ED has dropped by more than half, from 8.1 to 3.7 percent.
The program has since expanded to the ED at NYU Langone Health—Cobble Hill and to the Ronald O. Perelman Center for Emergency Services at Tisch Hospital. What’s more, as COVID-19 cases eased over the summer, 12 other common diagnoses were added to the discharge counseling roster, including back pain, headaches, urinary tract infections, and diabetes, each with an accompanying script to guide the students.
“We think this approach improves care, and we’re excited about building on it,” Dr. Wittman says.

