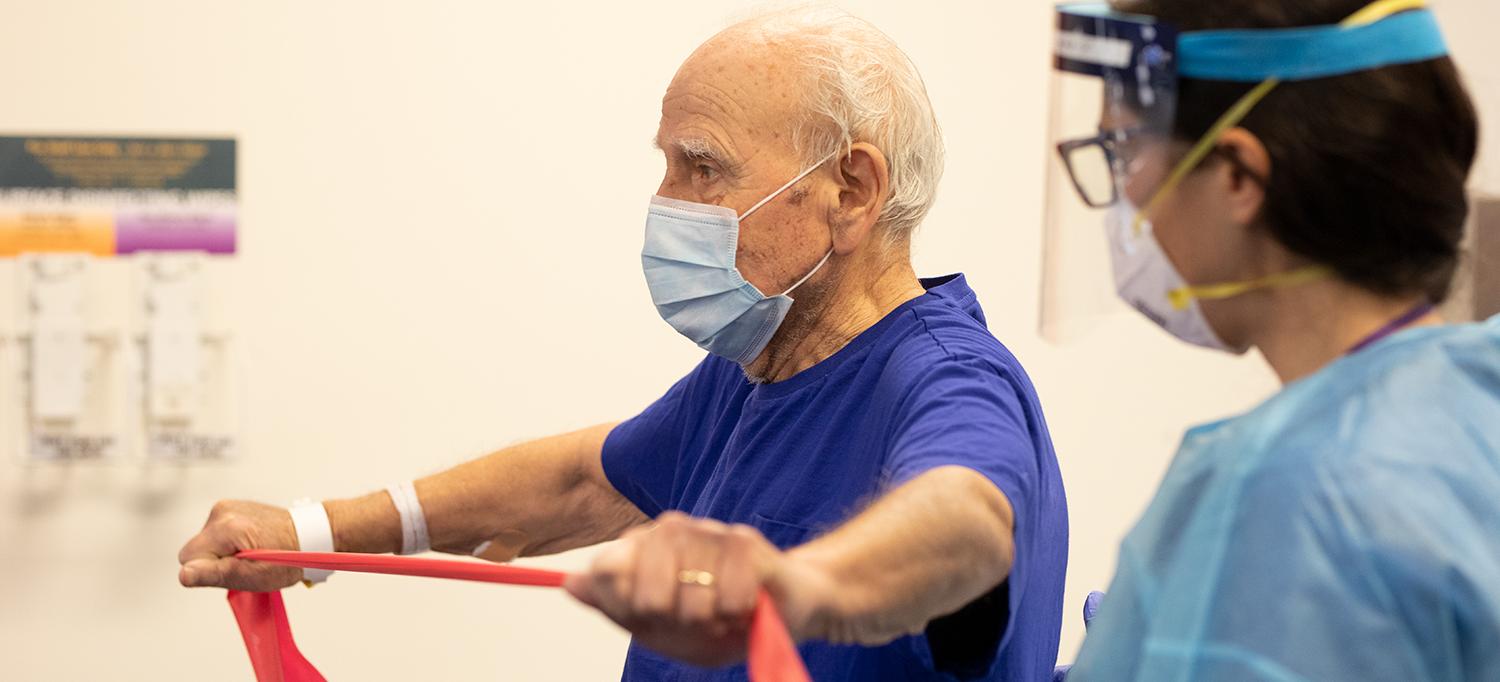
Rusk Rehabilitation’s multidisciplinary team quickly adapted to address the influx of patients with COVID-19, providing exceptional care in the rehabilitation unit and beyond.
Photo: Jonathan Kozowyk
When New York City became the U.S. epicenter of the coronavirus disease (COVID-19) pandemic in March, Rusk Rehabilitation at NYU Langone Health rapidly reconfigured its services to treat the flood of critically ill and recovering patients. Since then, Rusk Rehabilitation’s multidisciplinary team has continually adapted its approach to the evolving crisis.
Mobilizing for the Emergency
As caseloads began rising, leadership meetings were held daily to identify and address emerging needs across the medical center, with updates emailed to all faculty and trainees to enhance coordination. Rusk Rehabilitation’s two Manhattan-based inpatient rehabilitation facilities, at Tisch Hospital and NYU Langone Orthopedic Hospital, were repurposed within a week; one was reserved for patients recovering from COVID-19 and the other for patients who tested negative. Led by Jeffrey S. Fine, MD, associate professor of rehabilitation medicine and chief of the physical medicine and rehabilitation service at NYU Langone Hospital—Brooklyn, the inpatient rehabilitation facility at NYU Langone Hospital—Brooklyn was converted to an acute COVID-19 unit. “We quickly leveraged partnerships across multiple disciplines to manage a new acute medicine COVID unit, and subsequently a COVID recovery rehabilitation unit. Substantial operational changes were made to meet the needs of this patient cohort,” says Dr. Fine.
Although face-to-face outpatient visits were suspended to avoid the risk of contagion, virtual rehabilitation therapy through video visits was maximized, providing continuity of care for those who needed it most. Meanwhile, Rusk Rehabilitation’s research division engaged with numerous system-wide initiatives aimed at improving clinical and institutional approaches to pandemic-related challenges.
Providing Help Beyond the Rehabilitation Unit
Rusk Rehabilitation’s attending and resident physicians volunteered to treat patients with COVID-19 throughout the NYU Langone network. One important contribution was in prone positioning—a technique that has long been used to improve oxygenation in patients with acute respiratory distress syndrome and whose effectiveness for intubated patients with COVID-19 was first documented in late March in a study published in the American Journal of Respiratory and Critical Care Medicine. Patients on ventilators or with severely impaired mobility must typically be lifted and turned daily by teams of five or more clinicians and support staff.
At NYU Langone, proning teams were led by Rusk Rehabilitation physical therapists, in conjunction with acute care medical and nursing personnel. Rusk Rehabilitation clinicians also mobilized to provide a range of rehabilitation therapies to acute care services, including dysphagia management, early mobilization, and communication therapy.
Rusk Rehabilitation’s experience responding to prior public health emergencies, such as the 9/11 attacks and Superstorm Sandy, helped shape its initial response to the coronavirus crisis. “We carry this institutional memory in our culture,” says Alex Moroz, MD, MHPE, associate professor of rehabilitation medicine, vice chair for Rusk Rehabilitation’s education and training, and director of the Physical Medicine and Rehabilitation Residency. “When things get really difficult, our people just pull together and do what needs to be done.”
Responding Nimbly to Changing Conditions
The first wave of acute patients lasted approximately two months. “Early on, our team’s focus was on inpatient care,” explains Dr. Moroz. “The volume was very high, and we were all working incredibly hard to keep up with it.”
By late spring, Rusk Rehabilitation’s COVID-19–positive inpatient unit had begun to empty out, and the team’s clinicians were increasingly called upon to consult with other services whose patients with coronavirus had entered recovery. Finally, in June, Rusk Rehabilitation’s outpatient units were able to reopen, with a growing number of patients needing care for the long-term sequelae of COVID-19.
“This is a disease that affects every single organ system,” notes Jonathan H. Whiteson, MD, associate professor of rehabilitation medicine, vice chair for Rusk Rehabilitation’s clinical operations, and medical director of cardiac rehabilitation. “We’re seeing people who presented with respiratory failure and need pulmonary rehabilitation, people who’ve had strokes and need stroke rehabilitation, people who’ve had heart attacks and need cardiac rehabilitation. Many patients are struggling with a chronic post-viral fatigue syndrome, which we’re treating with lifestyle changes as well as exercise therapy and other modalities. We’re currently developing a comprehensive post–COVID-19 rehabilitation clinic to address these varied needs.”
Sharing Knowledge to Advance the Field
Rusk Rehabilitation’s unique perspective as a rehabilitation center amid the pandemic has received national and international attention through a series of webinars, directed by Dr. Moroz and hosted by Dr. Whiteson and Lyn D. Weiss, MD, professor of rehabilitation medicine and chair of the physical medicine and rehabilitation service at NYU Langone Hospital—Long Island, titled “COVID-19 Conversations: Powered by Rusk Rehabilitation.” These COVID-19–related lessons have also been shared through the Doctor Radio series on SiriusXM and through the podcast series Rusk Insights on Rehabilitation Medicine.
With a new wave of the pandemic now rising nationwide, Rusk Rehabilitation is prepared to step unto the breach once more. “I’m immensely proud of our team,” says Steven R. Flanagan, MD, the Howard A. Rusk Professor of Rehabilitation Medicine and chair of Rusk Rehabilitation. “Through their tireless work and dedication, they’ve helped improve COVID-19 outcomes and decreased the burden on acute care services throughout our hospital system—and beyond it.”

