Seeking Medical Care for Routine or Urgent Matters Is Safer Than Staying Home, Thanks to NYU Langone’s Rigorous COVID-19 Measures
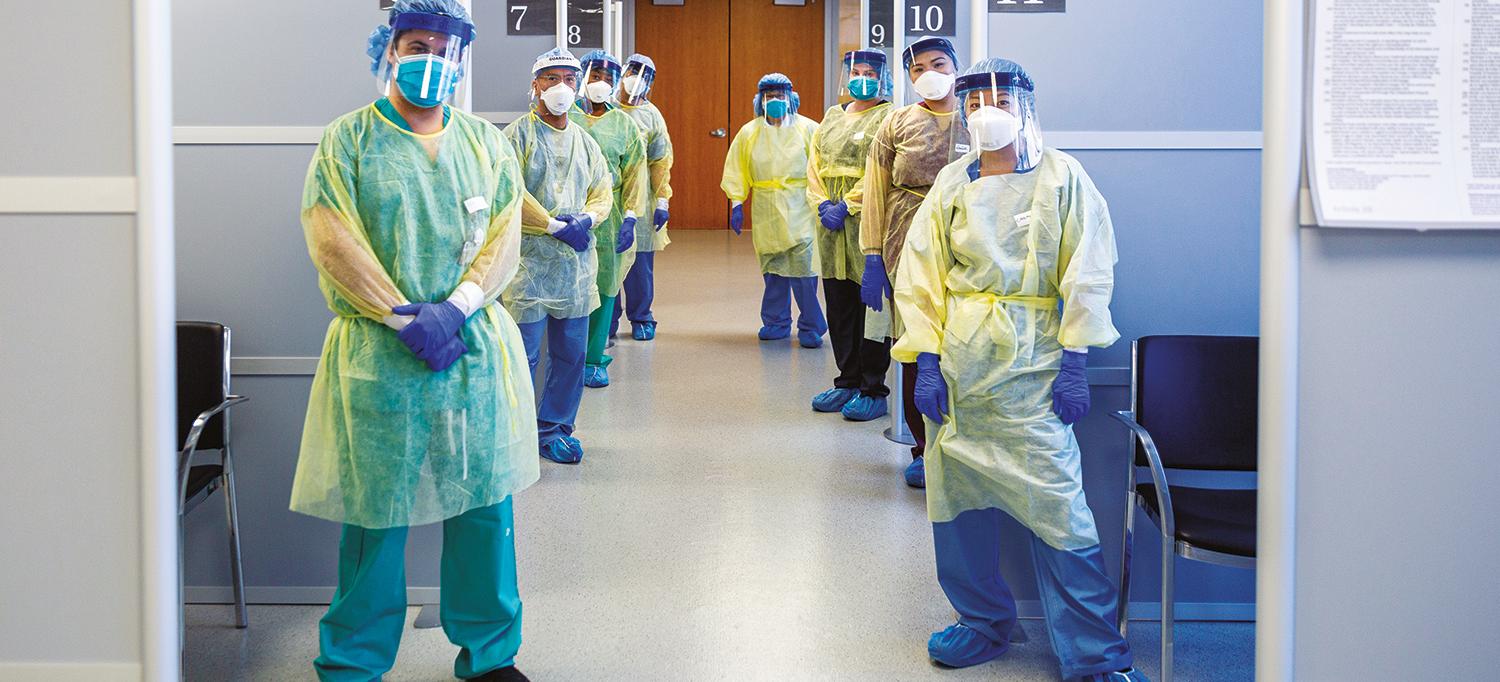
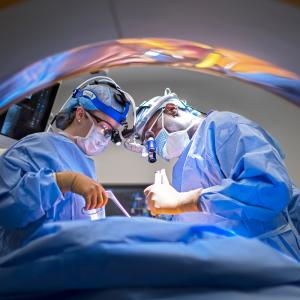
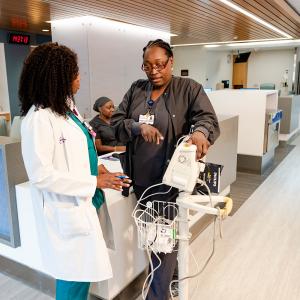
NYU Langone Health has taken every precaution to protect patients and prevent viral spread.
Photo: NYU Langone Staff
By the time the surge of spring infections abates in New York City, coronavirus disease (COVID-19) has sparked so much terror that people stay home even when they shouldn’t—in the midst of medical emergencies that threaten their lives. The U.S. Centers for Disease Control and Prevention (CDC) reported that in the 10 weeks after COVID-19 was declared a national emergency, visits to emergency departments nationwide declined by 20 percent for heart attack and stroke care and 10 percent for diabetic care. Between March 11 and May 2, New York City reported about 24,000 more deaths than usual during that period, and an estimated 20 percent of those mortalities were attributed to health issues unrelated to COVID-19.
The perception that visiting a hospital or doctor’s office poses a greater hazard than a supermarket or pharmacy has given rise to a secondary crisis: people neglecting their medical care or ignoring urgent warning signs. Mental health professionals say that’s just how the brain is wired. When we lack enough information to make plans or predictions confidently, anxiety can easily turn to dread. Last spring, emergency medicine physicians expected to see more heart attacks than usual, rather than fewer, due to intensified stress and the cardiac strain caused by COVID-19’s pulmonary damage. Other kinds of medical emergencies were also dangerously downplayed by patients. “When somebody has lower abdominal pain, which is associated with appendicitis, they usually come in to be seen,” says Andrew W. Brotman, MD, executive vice president, vice dean for clinical affairs and strategy, and chief clinical officer. “But during the first wave, we saw a 700 percent increase in the number of appendices that ruptured.”
Video visits and Virtual Urgent Care visits remain options when an in-person visit isn’t necessary or convenient. But face-to-face care is always best. Most patients have resumed routine screenings, such as colonoscopies, mammograms, and gynecologic exams, as well as annual physicals. In fact, by mid-July, the number of patient visits at NYU Langone Health’s faculty group practices was more than 100 percent higher than the pre-COVID-19 volume. At NYU Langone’s hospitals, emergency departments, and outpatient sites, rigorous measures have been implemented to ensure patient safety. “We’re taking extraordinary precautions to make sure our locations are as low risk as the can possibly be,” explains Andrew Rubin, senior vice president of clinical affairs and ambulatory care. “If you have to leave your house to go somewhere, this is the safest place to be.”