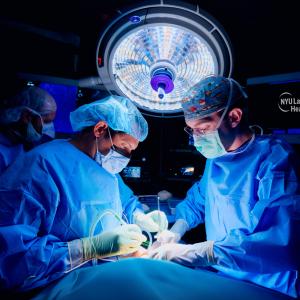
Photo: Taechit Taechamanodom/Getty
When David Lat was discharged on April 1, 2020, he was one of the first patients at NYU Langone to recover after becoming critically ill with 2019 coronavirus disease (COVID-19). It was a remarkable milestone for his medical teams, underscoring their collaborative efforts in caring for patients with severe COVID-19.
David was admitted on March 16 after developing fever, cough, and debilitating shortness of breath. He was hospitalized for 17 days, including 6 days when he was heavily sedated and connected to a ventilator to help him breathe. A healthy and active 44-year-old former marathon runner, David didn’t fit the expected profile of a patient with severe COVID-19.
For the hospital’s care teams, “that time was very emotionally challenging,” says hospitalist Luke F. O’Donnell, MD, who led the team of clinicians who cared for David before he was intubated. Dr. O’Donnell started seeing patients with COVID-19 the same week David was admitted. “The people we thought would be doing fine weren’t doing fine,” he recalls.
Without a standard treatment protocol, team members turned to experimental drugs and the expertise of colleagues as they confronted the previously unknown disease. They also banded together to help each other, offering mutual support and guidance to cope with the pressures of caring for a sudden influx of patients with severe illness.
Transforming a Hospital Unit
When David arrived at the Ronald O. Perelman Center for Emergency Services, the New York City–based journalist and legal recruiter was already experiencing respiratory difficulty. “Normally, I’d have walked the few blocks from my apartment to the hospital,” he says. “But at that point I could barely walk or stand.”
He was immediately given oxygen, and after receiving a positive COVID-19 test result, was admitted to the COVID-19 unit, known as KP12, on the 12th floor of NYU Langone’s Kimmel Pavilion. Only weeks before he arrived on KP12, the unit was dedicated to oncology and pulmonology. Adriana Quinones-Camacho, MD, medical director of KP12, and nurse manager Katie Weathers, RN, led the effort to transform the space into the medical center’s first dedicated COVID-19 unit.
Among the infrastructure changes was sealing each room and altering the ventilation to prevent air from being recirculated within the building. This change, putting each room on negative pressure, prevented the virus from lingering in the air.
Changes in staff and routines were more challenging. “Transitioning KP12 to the first COVID unit was a huge effort that involved a lot of teamwork and creativity,” says Dr. Quinones-Camacho. Teams were restructured and staff were reassigned from other floors and other duties. “We had to get the right people in to care for the patients.”
Collaboration with the infection prevention and control (IPC) team was vital, in particular as recommendations about personal protective equipment (PPE) were in flux. “It was a constant two-way conversation,” says Dr. Quinones-Camacho. “They were there to help guide us not just about how to set up the unit and care for the patients individually, but how we could best care for the staff.”
Group-Thought and Mutual Support
David spent five and half days on KP12. For the first 2, he was able to maintain his prodigious Twitter habit, sending dispatches to his nearly 33,000 followers, alerting anyone he’d been in contact with of his diagnosis and detailing his symptoms. “I’ve had 10 days & counting, with no real improvement, of fever, fatigue, joint aches, chills, cough, respiratory difficulty. I have never been this sick in my entire life,” he wrote in a March 17 tweet.
Despite not being able to see their son, David’s parents—both doctors—were able to speak to him and his care team. “Whenever a doctor came in, I could put my parents on speaker phone,” he says. “They could ask questions of my care team, and make recommendations, and just have peace of mind.”
Because there are no proven treatments for COVID-19, David’s team relied on rapidly evolving research-backed recommendations and the expertise of colleagues. “A lot of the decisions about the initial management came from group-thought,” says Dr. O’Donnell, whose team held a morning meeting with members of epidemiology, pulmonary intensive care, nursing, and others to discuss what they had been seeing and the best next steps for David and others with severe coronavirus disease.
Despite receiving supportive care and courses of the antiviral lopinavir–ritonavir and then a combination of the antimalarial hydroxychloroquine and the antibiotic azithromycin, David’s condition suddenly worsened on the evening of March 20. “We became very concerned that his body was tiring out and that he was starting to lose his fight against COVID-19,” Dr. O’Donnell says. “At that point we decided to intubate, and he was moved to the KP15 intensive care unit.”
It was a stunning setback not only for David, but also for members of his care team. “David was the very first patient I met on the COVID unit,” says Molly Forster, MD, one of the first NYU Langone residents to volunteer for COVID-19 duty. “Everything I read to prepare said that the patients would be older with comorbidities. David was extremely young and healthy. He was much sicker than I had expected him to be.”
To cope with the stress, the KP12 team relied on the support of colleagues, notably during the morning meetings. “It was very therapeutic to be with other people who were living the same experience as you and talking about it, but it was also uplifting because you knew you were involved in this huge group that’s taking care of people,” says Dr. O’Donnell.
While the medical team administered to David, social worker Elizabeth Janes, a member of the social work and care management services team, and staff chaplain Elizabeth Kitamura, a member of the spiritual care team, together phoned David’s husband, Zach Shemtob, to offer comfort and support.
Fortunately, Zach was coping well. “He had a lot of family and friends who were supporting him,” says Chaplain Kitamura.
A Thank You
David says he has only vague memories of being intubated and no recollection of the six days he spent on the ventilator in the intensive care unit (ICU). Heavily sedated, he was cared for by a team of nurses and doctors trained in ventilation management.
“I never heard his voice, but he made such an impression on me,” says Michele Pottberg, RN, who is back at work after a relatively mild case of COVID-19. “I could tell he had a fighting instinct.”
Gradually, David’s condition began to improve, and he required less and less oxygen. On March 26, his doctors decided it was time to extubate and remove him from the ventilator. Amanda Gallace, RN, was with him just before the procedure, as David was being weaned from sedation. “He was awake, but still pretty out of it,” she says. “He still had a tube in his throat.”
With a pen and pad, David wrote a message to her. “His writing was a bit scribbly, but I could make out, ‘Name?’ I told him, and then he wrote, ‘Thank you.’”
“It was my second week in the ICU, and he was the first patient who had done well. It was so beautiful. I’ll never forget it.”
After being extubated, David spent another week in the hospital, regaining strength. “Even after I was successfully extubated, it was still frightening,” he says. “I was scared by how weak I felt and how I could barely do—or sometimes just couldn't do —simple tasks like standing, walking, or going to the bathroom.”
But he continued to improve, and the supplemental oxygen he received was gradually reduced until he could breathe completely on his own. After another day of monitoring, David was released. Now home and on the mend, David thanks the people who helped him get well. “It’s all about the people at NYU Langone. They’re amazing. My care team was great at keeping up my spirits.”
NYU Langone’s frontline workers continue to bolster each other’s spirits during a crisis all are eager to see become just a memory. Nurse Michele Pottberg reflects on the challenge overcome by the institution during Superstorm Sandy.
“I worked the night Sandy happened,” she says. “I helped evacuate all the patients in the building. I will never forget it. We came back from that and we were stronger than ever. At some point in the future we’ll look back and say, wow, what a fantastic job everyone at NYU Langone did, and we’ll be bigger and better than ever, I’m sure of it.”