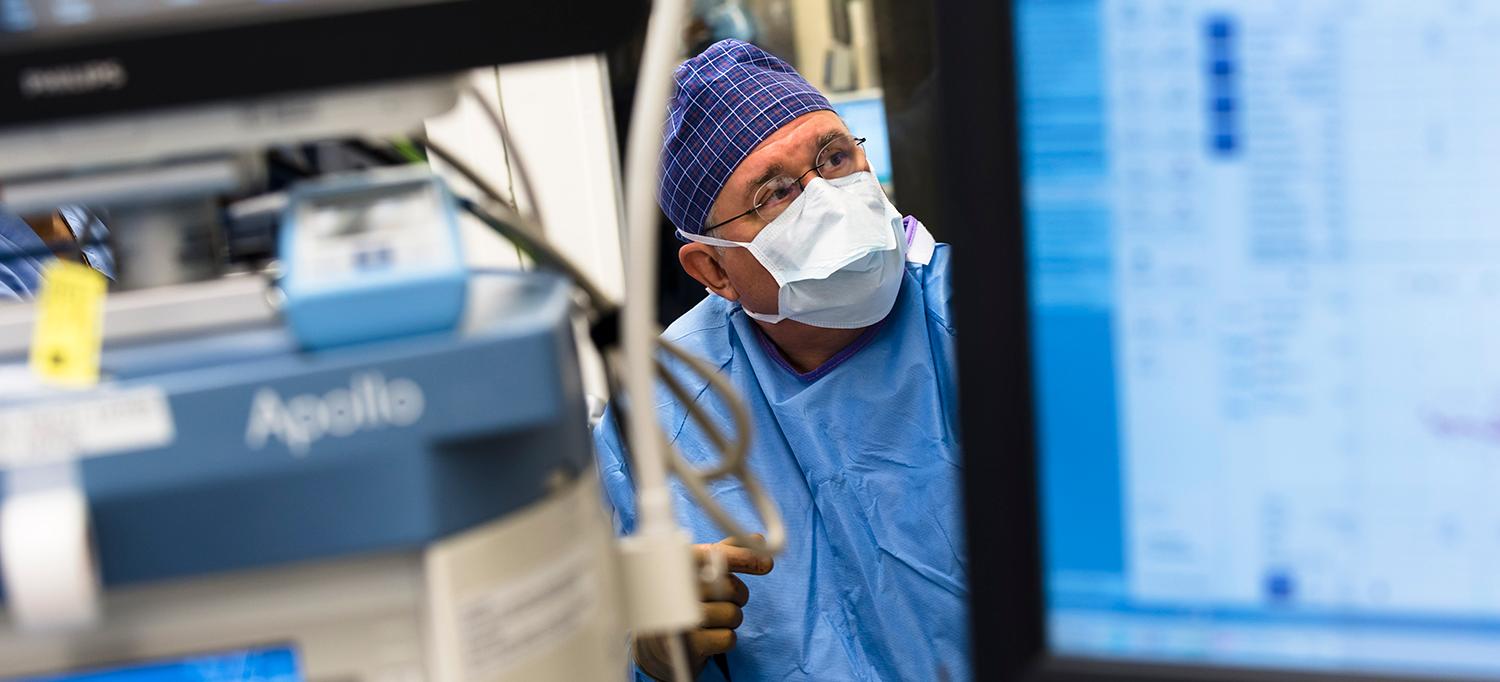
According to Cochlear Implant Center co-director Dr. J. Thomas Roland Jr., cochlear implantation using local anesthesia with sedation rather than general anesthesia may make the procedure available to a wider population.
Photo: Karsten Moran
With innovative techniques leveraging continually advancing research, clinicians at NYU Langone’s Cochlear Implant Center are uncovering greater potential for cochlear implants to enhance hearing, speech understanding, and quality of life for a larger number of patients.
Local Anesthesia Expands Access for Older Adults
Though there is evidence linking hearing loss with cognitive decline, it is estimated that only 5 percent to 7 percent of elderly adults who meet the criteria for cochlear implantation elect to receive one. One of several factors driving low adoption is research conflating general anesthesia and resulting post-operative dementia—prompting clinicians to pursue a solution.
Following the successful use of local anesthesia with sedation in a comorbid patient treated for an encephalocele, J. Thomas Roland Jr., MD, the Mendik Foundation Professor of Otolaryngology, chair of the Department of Otolaryngology—Head and Neck Surgery, and co-director of the Cochlear Implant Center, recognized that this same approach could avoid the risks of general anesthesia in cochlear implantation. He has used this method to implant approximately 80 patients since his first procedure in 2006.
Successful outcomes require nuanced expertise well-honed by experience, as well as expansive knowledge of the inner ear’s anatomy—limiting the availability of this approach to just a handful of specialized centers. The use of sedation demands that surgeons adhere to an accelerated procedural timeline, 40 percent faster than the traditional approach. They must also use caution in the delicate area near the facial nerve, remain in close communication with anesthesiology, and guide patients through the sensations experienced in real time in order to keep them comfortable and avoid voluntary movements.
These challenges notwithstanding, the use of conscious sedation in cochlear implantation has significant potential to improve treatment for elderly patients deemed too sick for general anesthesia, and Dr. Roland is hopeful that his work will empower other physicians to embrace this alternative. “It’s a safer approach that should become the standard of care, hopefully prompting more elderly people with hearing loss to consider cochlear implants, which can markedly improve their quality of life,” he says.
Artificial Intelligence Adds Objectivity to Cochlear Implant Programming
New research utilizing artificial intelligence (AI) in cochlear implant programming aims to apply objectivity to a process that has largely remained static over nearly three decades. NYU Langone is among a handful of nationwide centers participating in the clinical trial harnessing advanced technology, with the goal of delivering optimal functional performance for more patients.
Traditional programming is based on a combination of subjective patient feedback and programming expertise, with potential variability in efficacy due to differences in both the patient’s response and the audiologist’s device adjustments. “AI takes the guesswork out of programming,” says the study’s lead investigator, Susan B. Waltzman, PhD, the Marica F. Vilcek Professor of Otolaryngology—Head and Neck Surgery and co-director of the Cochlear Implant Center. “It gives patients the best possible chance of realizing the full potential of their implants by targeting optimal, objective performance and making that available to every patient, everywhere.”
Researchers are testing an AI technology called FOX, which uses psychoacoustic tests and other novel methods to calibrate patients’ devices to the appropriate pitch and volume. Sounds can be delivered directly from the audiologist’s computer to the device’s sound processor, enabling testing in a setting more natural than an audiometric booth. Since FOX measures individual results against a database of anonymous patient performance data to make unique fitting recommendations, outcomes should continue to improve as more information is integrated into FOX’s predictive technology.
Researchers plan to measure speech recognition improvements over six months for newly implanted patients participating in the trial; for existing devices, they will assess whether AI reprogramming improves outcomes. “Our hope is that AI will provide consistent access to the best possible programming, no matter where patients receive care,” says Dr. Waltzman.
Novel Electrode Placement Aims to Improve Cochlear Implant Performance
A new trial expands earlier NYU Langone cadaver-based research focused on optimizing the length and placement of cochlear implant electrodes.
Previous findings suggested that it is possible to stimulate lower-frequency auditory nerve fibers without deeper insertion of the electrode arrays. Since deeper insertion risks inner ear damage, the researchers explored methods to exploit greater levels of low-frequency information, finding that inserting a return electrode at the apex of the cochlea produces more even current distribution across channels. This, in turn, would be expected to improve cochlear implant users’ perception of low-frequency information, enhancing their ability to register music and high-quality sound. This research, just granted approval by the Institutional Review Board, will now move into human trials.
Five adults are enrolled in the initial pilot trial of this alternate technique utilizing the existing free ground electrode. Patients will undergo a series of tests postoperatively to gauge their perception of low-frequency information, to explore whether additional low-frequency information can be harnessed in live subjects without deeper electrode insertion. “We are stimulating areas designed to encode for low frequencies, which are ignored in most implant systems,” says Dr. Roland. “It’s a groundbreaking way to get more from existing technology simply by utilizing an electrode that’s already there.”