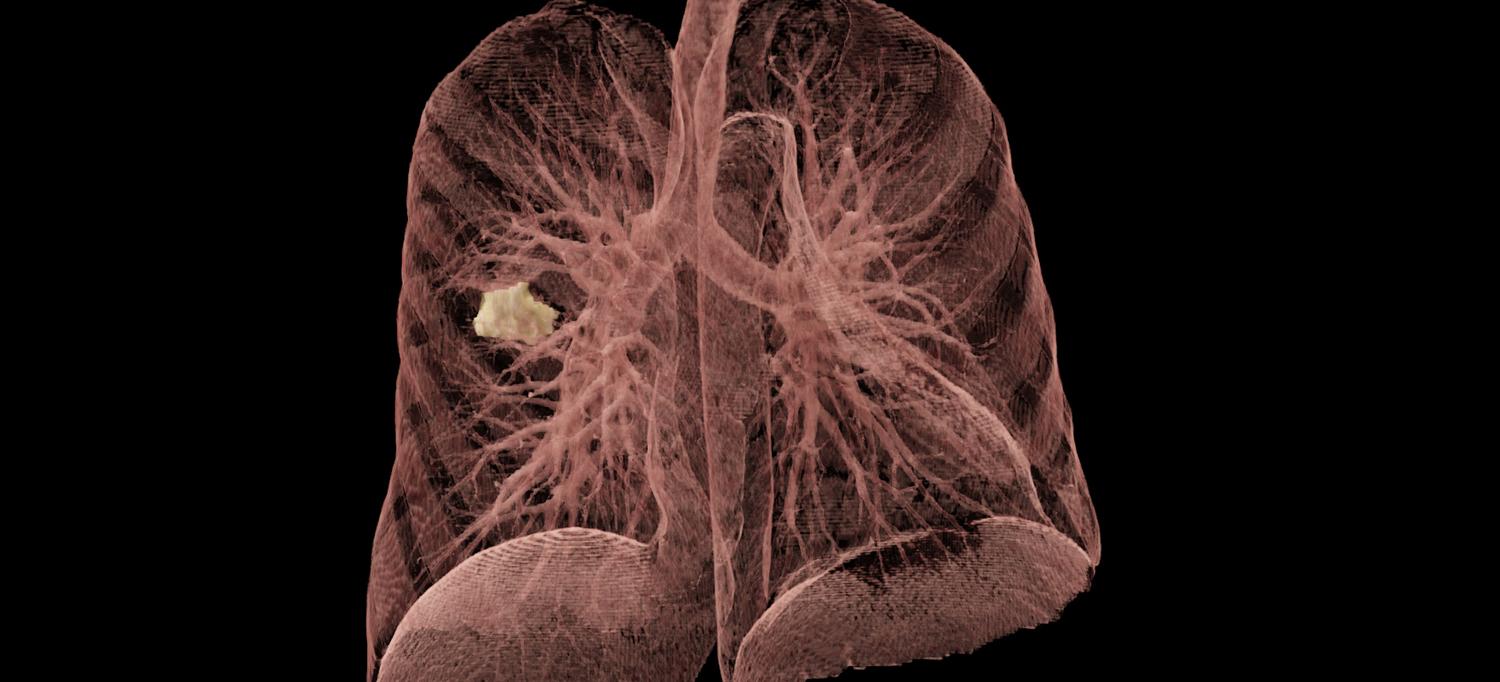
A three-dimensionally rendered image of a low-dose CT chest scan, performed during a routine lung cancer screening at Perlmutter Cancer Center, reveals a tumor in a patient’s right lung.
IMAGE COURTESY NYU LANGONE RADIATION TECHNOLOGIST DAWN-MARIE SWAHN AND WILLIAM H. MOORE, MD, PROFESSOR OF RADIOLOGY
In his role as medical director of NYU Langone’s Lung Cancer Center, Abraham Chachoua, MD, has seen significant improvements in the treatment of a dreaded disease once thought of as a death sentence. A new generation of therapies harnesses the power of the body’s immune system to kill off tumor cells, while others target specific molecules to block the growth and spread of cancer cells. All told, NYU Langone’s Perlmutter Cancer Center offers more than 30 clinical trials of investigational therapies for lung cancer.
Meanwhile, for lung cancer caught in its earliest stages, major advances in robotic thoracic surgery allow surgeons to excise a small section of the affected lung rather than an entire lobe. In effect, patients leave the operating room cured. Altogether, the wave of progress has helped physicians at the Lung Cancer Center extend the lives of many of the 1,200 patients they treat annually.
Despite these impressive advances, the prognosis for most patients with lung cancer remains poor. The aggregate 5-year survival rate is just 25 percent, according to the American Cancer Society, and some 132,000 people die from lung cancer each year, twice as many as from any other cancer. The problem is that lung cancer rarely becomes symptomatic until the disease has advanced and spread to other parts of the body.
For this reason, Dr. Chachoua sees early detection as a critical lifesaving intervention. Annual screenings for lung cancer have been found to reduce mortality among smokers by 20 percent, according to results from the National Lung Screening Trial, sponsored by the National Cancer Institute (NCI), which studied more than 50,000 current or former heavy smokers. Unfortunately, only about 2 percent of eligible patients receive them.
“We still can’t cure lung cancer, with the exception of a very small number of patients,” says Dr. Chachoua, the Jay and Isabel Fine Professor of Oncology. “The best way is to catch it early and remove it.”
That’s precisely the idea behind two major screening initiatives at Perlmutter Cancer Center, an NCI-designated Comprehensive Cancer Center. The first is the expansion of the Lung Cancer Screening Program to locations throughout Manhattan, Brooklyn, Queens, and Long Island, for patients who are eligible based on their smoking history. Since its launch last year, more than 250 patients identified through NYU Langone’s electronic health record system have begun receiving annual low-dose CT chest scans, which can often detect cancer at an early stage.
“A lot of people don’t realize that up to 20 percent of those diagnosed are nonsmokers, or that patients in this group tend to be diagnosed at younger ages, often in their 40s or 50s.”—Elaine Shum, MD, Medical Oncologist with Perlmutter Cancer Center
The second project is a major study, led by principal investigator Elaine Shum, MD, medical oncologist and assistant professor in the Department of Medicine at NYU Grossman School of Medicine, that intends to shed light on why Asian American women are disproportionately affected by lung cancer. Some 40 percent of Asian American women diagnosed with the disease are nonsmokers, at least double the rate of the general population. While a number of possible links have been suggested, including exposure to cooking oil fumes, secondhand smoke, and a genetic predisposition, none have been confirmed as causes. “That’s the $64,000 question we want to answer,” says Dr. Chachoua.
Dr. Shum says researchers have long been aware of a strong connection between nonsmoking Asian women and a common lung cancer mutation of the epidermal growth factor receptor, or EGFR, causing abnormal cell growth. Yet few studies have examined the factors that might explain it.
Perlmutter Cancer Center has begun enrolling Asian American women ages 40 to 74 who have never smoked or have smoked fewer than 100 cigarettes in their lifetime, and who have no history of cancer. During the three-year study, volunteers will receive an annual low-dose CT scan of the chest while donating a blood sample for an experimental screening tool that uses machine learning to detect genetic markers of seven types of cancer. The study’s topline goals are to create a database, collect biospecimens, and identify risk factors. In addition, Dr. Shum hopes to debunk the myth that lung cancer is only a smoker’s disease. “A lot of people don’t realize that up to 20 percent of those diagnosed are nonsmokers, or that patients in this group tend to be diagnosed at younger ages, often in their 40s or 50s,” says Dr. Shum.
While the Lung Cancer Center’s screening program provides scans for those who are uninsured or underinsured, Dr. Chachoua is optimistic that this latest study will help shore up the case for expanding health coverage of lung cancer screenings to nonsmokers as well as smokers. “This could potentially be a practice-changing study that opens up screening to people who don’t smoke,” he says. “There’s definitely a need for it.”
Patients interested in learning more about the New York Female Asian Nonsmoker Screening Study or enrolling can call 212-731-6212 or email fanss@nyulangone.org.

