NYU Langone’s Success in Treating Dire Cases of COVID-19 with a Last-Resort Intervention Rewrites the Rules

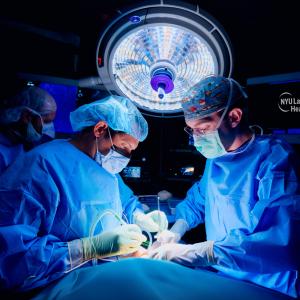
Bridget Toy, the program manager of ECMO and mechanical circulatory support, and Amy Emmarco, a mechanical circulatory support clinical resources nurse, trained 145 nurses in caring for patients on ECMO during the spring COVID-19 surge.
Photo: Jonathan Kozowyk
On April 8, 2020, Brian Hamdan, an 18-year-old high-school senior from Bronxville, New York, headed home after spending nearly a month in an intensive care unit at NYU Langone’s Tisch Hospital. Hamdan’s recovery was nearly as swift as his decline one month earlier from coronavirus disease (COVID-19) had been. At one point, Hamdan’s lungs were so ravaged by inflammation that they were unable to absorb the oxygen flowing from a ventilator, even when it was dialed to the highest settings. As his carbon dioxide levels began to spike, his doctors intervened early with a form of life support that does what the lungs no longer can: pumps oxygen into the blood while filtering out the excess CO2. The technique, a form of extracorporeal membrane oxygenation, or ECMO, serves as a mechanical gas exchanger, allowing the ventilator to be dialed down to a gentle setting so the lungs can heal.
While ECMO was used with some success in 2009 to treat severe cases of H1N1, early data on its usage in COVID-19 patients had been sparse, and mostly discouraging. One study of 17 patients reported a mortality rate of 94 percent. In stark contrast, NYU Langone’s rate is under 4 percent, thanks in part to a multidisciplinary approach that favors early intervention. “The longer you’re on a ventilator before ECMO, the worse the outcome,” says cardiothoracic surgeon Zachary N. Kon, MD, surgical director of NYU Langone’s Lung Transplantation Program. “The earlier we get to a patient, the better. Minimizing injury to the lungs from the ventilator is important.”
Under ordinary circumstances, the ECMO team in Manhattan performs more than 80 procedures a year. About half of those are for patients with severe lung conditions. By mid-June, the team had already placed 30 COVID-19 patients on ECMO. Twenty-one patients had improved enough to come off the machine, and all but two patients had survived. What’s more, none of the clinical staff developed symptoms or tested positive for COVID-19. “These outcomes are among the best in the world for COVID patients,” says cardiac surgeon Deane E. Smith, MD, director of the ECMO Program at Tisch Hospital.
The ideal candidate, NYU Langone experts have found, has failed to respond to the ventilator and stands a good chance of surviving if their lungs have time to heal. This often means younger patients whose organs remain healthy.
Taking the ECMO approach one step further, NYU Langone physicians began using the machine to filter out the cytokine proteins floating in blood that might spark an immune attack known as a “cytokine storm.” The filter has been used with some success to treat sepsis, but little is known about its potential benefits to COVID-19 patients.
Nader Moazami, MD, surgical director of the Heart Transplant Program, received emergency clearance from the U.S. Food and Drug Administration (FDA) to add an in-line filtration system to the ECMO machines at NYU Langone. He has collaborated with cardiothoracic surgeon Harvey I. Pass, MD, to evaluate the cytokines associated with COVID-19 and to study gene expression in ECMO patients.
“This type of aggressive clinical approach, combined with sophisticated scientific analysis, can only be done in a major academic medical center,” notes Aubrey C. Galloway, MD, chair of the Department of Cardiothoracic Surgery. “Our team feels our current approach will have a real benefit for our patients—and we aim to have the scientific evidence to back it up.”