Smallpox. Polio. Yellow Fever. HIV. NYU Langone’s Courageous Front Line Builds on a Long & Vibrant Legacy of Helping New Yorkers Shoulder Deadly Epidemics.
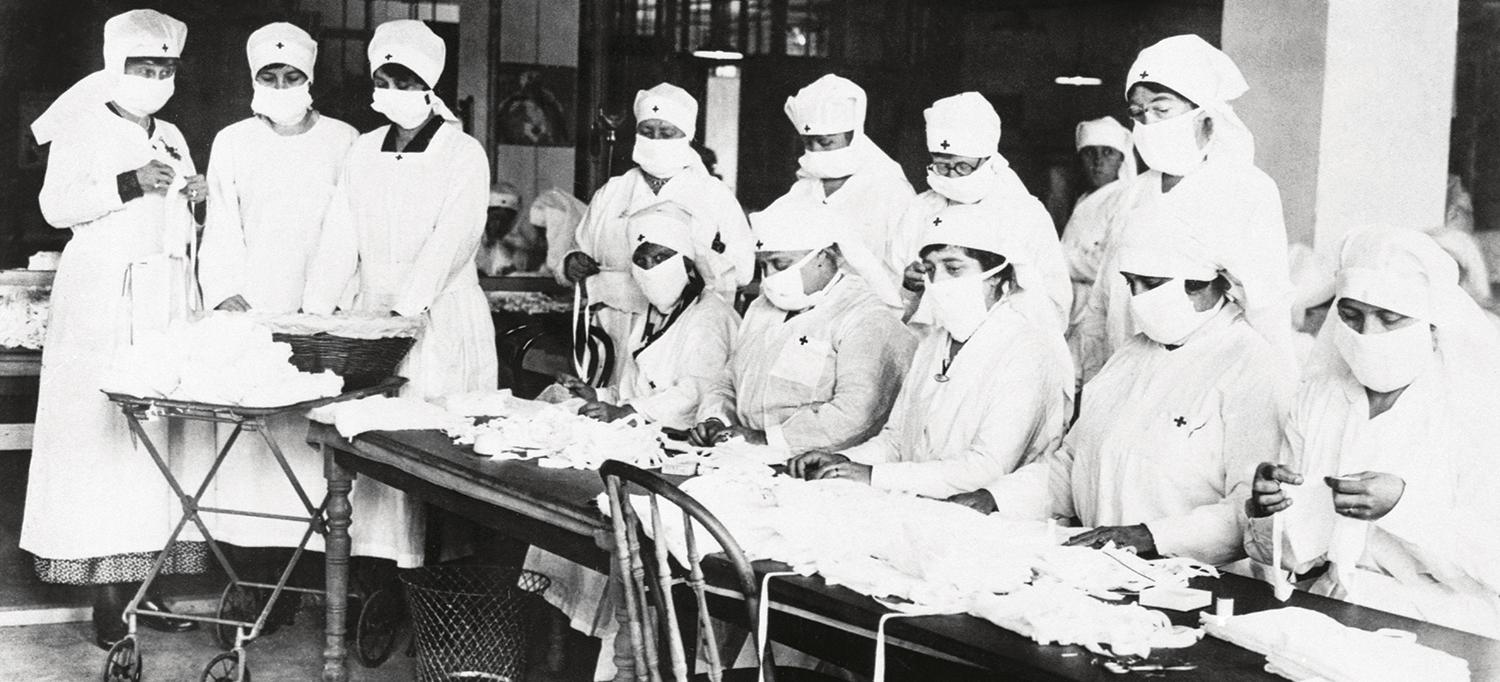
During the 1918 influenza pandemic, face masks—shown being made by American Red Cross workers—were a critical containment tool.
Photo: Bettmann Archives/Getty Images
Families huddled around radios as if listening to the World Series or a championship fight. Crowds stood four deep on city sidewalks watching the TV sets placed in department store windows. Loudspeakers blared out the news in offices and on factory floors: “The vaccine works. It’s safe, potent, and effective.” To many, April 12, 1955, resembled V-J Day—the end of a war. “Outside, we could hear horns honking and church bells chiming in celebration,” a fourth-grader from Baltimore recalled. “We had conquered polio.”
It hadn’t been easy. The struggle took more than two decades, culminating in the largest public health experiment in American history. More than a million schoolchildren participated, some getting the real polio vaccine, others a look-alike placebo. Today, the scourge of polio is a distant memory in most parts of the world, thanks to the killed-virus vaccine developed by Jonas Salk, MD, and the live-virus version championed several years later by Salk’s competitor, Albert Sabin, MD. As so often happens in bitter rivalries, the two men held many things in common—none more precious than the diplomas they earned from NYU Grossman School of Medicine.
The story of the polio vaccine—like so much else in the conquest of epidemic disease—has deep roots at NYU Langone Health. Had our medical school not existed, Jonas Salk, MD, and Albert Sabin, MD, would likely have chosen different careers.
The story of the polio vaccine—like so much else in the conquest of epidemic disease—has deep roots at NYU Langone Health. Had our medical school not existed, Salk and Sabin would likely have chosen different careers. As the children of Jewish immigrants, they gravitated to one of the few places that didn’t have a “Jewish quota.” (“Never admit more than five Jews, take only two Italian Catholics, and take no blacks at all” was the mantra of at least one Ivy League school.) A few years later, when applying for a fellowship that would start him on the road to the polio vaccine, Salk needed the blessing of his NYU mentor, Thomas Francis, MD, a giant in the field of infectious disease. Realizing that the process had as much to do with religion as with talent, Francis ended his recommendation with these carefully chosen words: “Dr. Salk is a member of the Jewish race but has, I believe, a very great capacity to get on with people.”
The medical education of Salk and Sabin speaks volumes about NYU’s early leadership in virology, bacteriology, and infectious disease. While elite institutions like Harvard and Johns Hopkins received the lion’s share of attention, NYU had compiled a record to match—more quietly, perhaps, but no less impressive.
Salk readily admitted his debt to R. Keith Canaan, PhD, a brilliant biochemist who recruited the young medical student to work in his laboratory, and to Francis, whose pursuit of a killed-virus flu vaccine would deeply influence Salk’s research agenda. Indeed, the caption under Salk’s 1939 NYU graduation photo read: “Seems to have researched in every laboratory on First Avenue … Can probably call more faculty members by their first name than anyone in school.”
Sabin’s NYU experience proved equally rewarding. As a first-year medical student in 1926, he caught the eye of the influential William Hallock Park, MD, who had introduced the lifesaving diphtheria antitoxin to America’s medical community. Park had been at NYU since 1900, serving as a department chair and then dean of the medical school.
Working in Park’s laboratory, Sabin developed a method for the rapid typing of pneumococci. Park proudly called it “the Sabin method” and claimed that it saved lives. As with Francis and Salk, the relationship between Park and Sabin exemplified the generational partnerships that fueled the extraordinary research occurring at NYU. “He was my champion,” Sabin recalled, “the illustrious, gentle, and warm-hearted Dr. Park.”
New York City’s Battle Against Numerous Epidemics
It takes the fear of a pandemic, as we are experiencing today with coronavirus disease (COVID-19), to remind us that epidemics have long marked our history. No American city suffered more than New York, whose bustling harbor became a magnet for the world’s microbes and maladies. Periodic eruptions of measles, influenza, cholera, and scarlet fever killed untold numbers in the colonial era, especially children. Barely a decade went by without a serious outbreak of smallpox—the epidemic of 1731 causing 500 deaths in a city of barely 10,000 people. Then, in the 1790s, came the scourge of yellow fever, causing the city fathers to buy a decaying mansion overlooking the East River to house the sick and dying—the “Bel-Vue Estate.”
Nobody at this time knew what caused yellow fever or how to treat it. Physicians blamed the disease—indeed, virtually all diseases before the acceptance of germ theory—on dangerous airborne clouds known as miasmas. The favored treatments for yellow fever were purging and bleeding, which did nothing but add to the pain. The only good news was that those who survived were immune for life.
A young doctor named Alexander Anderson, MD, faced the epidemic virtually alone. Barely into his 20s, he had left his family to treat the sick who arrived at Bellevue by horse cart and river barge. “We lost three patients today,” reads an entry in the remarkable diary he kept. “I am sometimes tempted to resign my station, but, really, I am afraid that like Jonah, I shall meet a worse fate.” In the summer of 1798, Anderson’s infant son died of yellow fever. In September, the disease took his brother, then his father. In October, it claimed his wife and his mother. “A tremendous scene have I witnessed,” reads Anderson’s final diary entry, written on New Year’s Eve. “Yet I have reason to thank the Author of my existence and am still convinced that ‘whatever is right, is right.’ ” For Anderson, being right meant taking responsibility for society’s most fragile members. Forgotten today, he stands as Bellevue’s first true physician, serving a riverfront pesthouse in a murderous time.
The link between these two institutions goes back to 1841, when the NYU College of Medicine first opened its doors, and Bellevue quickly became its training ground.
Fast-forward a full century to the work of Walter Reed, MD, and William Gorgas, MD, the clinician/researchers who unlocked the mysteries of yellow fever—the former demonstrating its transmission (the vector being the Aedes aegypti) and the latter providing the first blueprint for its eradication (draining swamps, screening windows, fumigating with wood alcohol). Their work not only lowered the casualty rates in the Spanish-American War, it also aided construction of the Panama Canal. Many consider their contributions to be among the most significant in the history of medicine. Fittingly, both men had been trained and educated at Bellevue and NYU.
The link between these two institutions goes back to 1841, when the NYU College of Medicine first opened its doors, and Bellevue quickly became its training ground. The partnership would survive some intense crises—none more severe than the epidemic of 1848, when typhus struck New York City. A bacterial disease spread by a body louse, it likely came from Europe on the so-called “famine ships” carrying Irish immigrants to the East Coast port cities of the United States. As the sickness spread, Bellevue erected “pest tents” to handle the overflow. The patient death rate soon exceeded 40%, and for the staff, it was even higher. So many resident physicians fell to the disease that medical students were used to fill the void. There is no record of anyone fleeing. To scroll through the fatalities of this epidemic is akin to reading the names on a war memorial:
- Elihu Hedges, student of medicine, died in NYC, 1848. Cause: typhus fever, contracted while on duty in the hospital.
- Gorham Beals, MD, died in NYC, 1848. Cause: typhus fever, contracted while on duty in the hospital.
- David Seligman, student of medicine, died in NYC, 1848. Cause: typhus fever, contracted while on duty in the hospital.
- William Cahoon, MD, died in NYC, 1848. Cause: typhus fever, contracted while on duty in the hospital. The list, comprising dozens of names, is a reminder of those who selflessly walked our halls long ago.
The Role of NYU Physicians in Developing TB Treatments
In 1870, 20 percent of the children born in New York City would not live to see their first birthday, and 25 percent of those who did reach adulthood would die before the age of 30. Many perished in the terrifying epidemics that periodically swept the region, but many more fell to endemic diseases related to filth and overcrowding—in short, the plagues of modern city life. Among the deadliest offenders was tuberculosis.
NYU Physician Herman Biggs, MD, lobbied for quarantine, facial masks, and the mandatory reporting of all suspected TB cases, followed by a sputum culture—a process opposed by most doctors at the time. Biggs prevailed.
The battle to contain TB in the late 19th and early 20th centuries owed its success to a cadre of NYU physicians, most notably Hermann Biggs, MD, and Edith Lincoln, MD. Guided by the microscopic isolation of the tubercle bacillus in 1884, Biggs used his funding as the head of New York City’s Medical Research Laboratory to lobby for quarantine, facial masks, and the mandatory reporting of all suspected TB cases, followed by a sputum culture—a process opposed by most doctors at the time as a threat to their livelihood. Biggs prevailed. “Public health is purchasable,” he famously declared.
Though close to half the patients in Bellevue’s sprawling chest unit were children, it didn’t create a special ward for them until the 1920s, when Lincoln, an assistant professor of pediatrics at NYU, took the job. (Earlier, as one of the first female interns at Bellevue, she had refused to eat with the nursing staff, demanding, and winning, a seat in the doctors’ dining room. As payback, she was warned for wearing her skirts too high.) A disciple of Biggs and his preventive methods, Lincoln compiled data for one of the largest medical studies of that era, tracking close to 3,000 TB survivors from the time they entered her ward until their 25th birthday. Her conclusions reinforced the work of most social reformers: the patients, almost without exception, “came from low socioeconomic backgrounds.” Nearly half of them were black and Puerto Rican at a time when their combined percentage in Manhattan was below 20 percent.
In the mid-1940s, Selman Waksman, PhD, a microbiologist at Rutgers, revealed that a soil-based derivative he called streptomycin had shown great potential in killing the tubercle bacillus. While testing it at Bellevue, Lincoln achieved even better results by using streptomycin in combination with a second antibiotic, isoniazid, which lowered TB mortality in the children’s ward to 1.5 percent—a success rate confirmed in later trials by the US Public Health Service.
Today, Biggs is considered by many to be “the father of public health in the United States.” Waksman went on to win the 1952 Nobel Prize in Medicine. Lincoln never received the acclaim she deserved, though her studies of multidrug therapies would reorient the treatment for tuberculosis—and later, some believed, for HIV/AIDS. Her true reward, she said, lay in watching her once-jammed TB ward empty out and eventually close. For NYU’s Lincoln, that legacy seemed more than enough.
The Two Past Health Crises That Most Resemble COVID-19’s Impact
If historical comparisons are to be made regarding the impact of COVID-19, two examples stand apart. Nothing in modern times comes close to matching the fury and devastation of the “Great Influenza” of 1918 or the decades-long struggle against HIV/AIDS. The influenza pandemic of 1918 killed more people in a shorter period than any event in world history. At least 50 million perished, including 700,000 in the United States—a number so staggering that the life expectancy of the average American dropped by 12 full years.
As the virus spread, the New York City Health Department banned spitting as well as “promiscuous coughing and sneezing.” To prevent crowding, work hours were staggered, and theaters were forced to cut their ticket sales in half. Public libraries stopped lending books, gauze face masks became regular attire, and people stopped shaking hands.
Bellevue saw more admissions in the fall of 1918 than at any time in its history. There was little to be done beyond providing aspirin, whiskey, and words of comfort. So many nurses and doctors took sick that city officials thought seriously about refusing new patients; they decided against it, though many wound up sleeping on the floor. “It got to the point where I would see them only twice,” a medical resident recalled. “Once when they came in and again when I signed their death certificate.”
New York City had a lower death rate from the Great Influenza of 1918 than Boston or Philadelphia. Early intervention worked; so, too, did social distancing, the banning of large public events, and a layered approach to reopening the city—painful lessons that resonate to this day.
Meanwhile, work proceeded on a flu vaccine, led by Biggs and Park. The results proved discouraging. Their laboratory couldn’t isolate the responsible pathogen, an impossible task given the mysteries of the endlessly mutating virus. In the end, an estimated 30,000 New Yorkers perished in the pandemic. Still, the city could boast a significantly lower death rate than Boston or Philadelphia due to the active involvement of its public health officials, led by the ubiquitous Biggs. Early intervention worked; so, too, did social distancing, the banning of large public events, and a layered approach to reopening the city—painful lessons that resonate to this day.
Unlike previous epidemics that ravaged New York City, AIDS had no history, not even a name, when it first appeared in the fall of 1980. NYU’s Fred T. Valentine, MD, saw his first case at Bellevue in the form of pneumocystis pneumonia, a rare opportunistic infection, while Alvin Friedman-Kien, MD, saw his first case at NYU Dermatology Clinic in the form of Kaposi’s sarcoma, an equally rare skin cancer. The only visible link was that both patients were gay men in their 20s with severely compromised immune systems. Before long, the net had widened to include drug addicts sharing needles and hemophiliacs receiving blood transfusions. Were they all suffering from the same disease? If so, how was it transmitted? With death being the one certainty, panic was palpable.
A decade earlier, the medical schools at Cornell and Columbia had departed Bellevue, leaving the hospital’s entire medical needs in the hands of NYU. Then came the pandemic. More patients would be treated for AIDS at Bellevue, and more would die, than at any other hospital in the United States. Gowns, face masks, double gloves, and goggles became standard equipment for doctors and nurses on the AIDS floors, though many abandoned the attire once the mode of transmission became known. Those who worked and trained at Bellevue in those years recall a sense of bonding and accomplishment that framed their later professional lives. They also remember the feelings of futility that often overwhelmed them in early years of the epidemic. “Every third admission seemed to be a patient in his mid-20s who looked as if he arrived from Dachau or Biafra,” a resident confessed. “Witnessing your own generation dying off is not for the faint of heart.”
By the 1990s, two groups affiliated with NYU had begun testing a multidrug therapy designed to suppress HIV in already infected patients—one group led by David Ho, MD, the other by Valentine. Both showed promising results. The viral loads of the subjects dropped to almost undetectable levels and stayed there as long as the routine was faithfully followed. By the year 2000, Bellevue was seeing more AIDS patients in its outpatient clinics than on its wards, and in 2012, the hospital shuttered its AIDS unit, a once unthinkable move. A momentous chapter in the history of NYU and Bellevue had closed—perhaps for good.
A History of Meeting Health Challenges Head on
The COVID Army called to duty over the past few months is part of a tradition spanning two centuries. Crises erupt, and professionals rise to the challenge.
From the indomitable Alexander Anderson to the young physicians who sacrificed their lives in the typhus epidemic of 1848, from the brilliance of Salk and Sabin to the selflessness of the frontline AIDS fighters—that is our history, refreshed by each succeeding generation.
About the Author
Historian David M. Oshinsky, PhD, is the director of the Division of Medical Humanities and Professor in the Department of Medicine at NYU Grossman School of Medicine. His books include Polio: An American Story, which won the Pulitzer Prize for History in 2006. His essays and reviews appear regularly in The New York Times and other publications.

