After 11 Months in the Hospital, Aydin Celebrates 1st Birthday at Home with Family

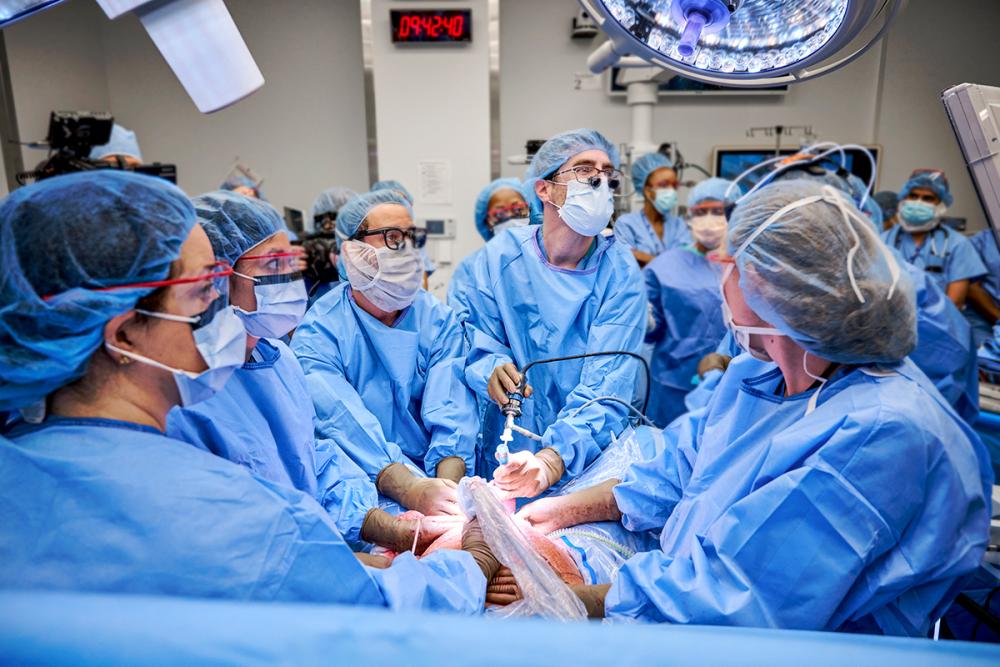
Yadi and Jamaal Martin credit the care team at NYU Langone, including maternal–fetal medicine specialist Dr. Ashley S. Roman and pediatric surgeon Dr. Jason C. Fisher, with saving the life of their son, Aydin.
Photo: James Yarusinsky
Aydin Idris Martin, an infant with an extremely rare and serious birth defect, was saved at birth when a multidisciplinary team at Hassenfeld Children’s Hospital at NYU Langone performed a highly specialized procedure.
The procedure was the first step in his journey to survive congenital high airway obstruction syndrome (CHAOS), a condition that inhibits an infant’s ability to breathe at birth. After 169 days in the Neonatal Intensive Care Unit at Tisch Hospital (NICU), followed by more than 5 months in a rehabilitation facility overcoming further challenges linked to CHAOS, Aydin is finally home with his parents Yadi and Jamaal Martin to celebrate his 1st birthday.
Multimedia Materials Available
Multimedia materials, including photos, B-roll package, and interviews with clinical experts and family, are available for download.
A Prenatal CHAOS Diagnosis
CHAOS is a congenital condition that occurs when the trachea, also known as the windpipe, is blocked or not fully formed during fetal development. The condition, whose causes remain unknown, comes with a 100 percent mortality rate unless an intervention is performed at birth.
The Martins received the diagnosis in May 2021, 24 weeks into Yadi’s pregnancy. A fetal echocardiogram that showed abnormalities led James C. Nielsen, MD, medical director of the Pediatric Congenital Heart Program at Hassenfeld Children’s Hospital, to consult with Ashley S. Roman, MD, vice chair for clinical affairs for obstetrics, co-director of the Fetal Diagnosis and Treatment Program, and director of the Division of Maternal–Fetal Medicine in the Department of Obstetrics and Gynecology at NYU Grossman School of Medicine. She instantly confirmed the diagnosis of CHAOS.
VIDEO: Learn more about the Martins’ journey at NYU Langone and the highly specialized delivery method that allowed them to welcome their first child into the world.
“The ultrasound revealed large, overinflated lungs, and I immediately knew what was wrong,” says Dr. Roman. Yadi’s unborn child was only the second she had seen with CHAOS in her career of over 20 years, and the 51st case publicly reported in the United States since 1989. “As a result of the airway blockage, the lung fluid cannot escape the fetal mouth, causing the lungs to fill up immensely and swell. The condition would make breathing impossible and fatal for the baby after a traditional delivery.”
After four prior miscarriages, this was not the news the couple hoped to hear almost halfway through their pregnancy. “This was our miracle baby,” Yadi says. “We prayed and prayed for him.”
“As soon as we learned of the diagnosis, we initiated a multidisciplinary team to begin the months of preparation needed to ensure that everything went smoothly in the delivery room,” says Jason C. Fisher, MD, pediatric surgeon, director of children’s surgical services for Hassenfeld Children’s Hospital, and director of the Division of Pediatric Surgery at NYU Grossman School of Medicine. “When you have a case of such complexity, you can’t do it alone. You need to have a medical center that offers all these subspecialists in one setting, and that’s Hassenfeld Children’s Hospital at NYU Langone.”
Instead of a traditional birth, Aydin required an innovative surgical approach called ex utero intrapartum treatment, or EXIT, that would establish an airway before he was separated from the placenta.
“The most important thing about CHAOS is early diagnosis, detailed fetal assessment, and an adequate postnatal intervention for establishing an airway,” says pediatric head and neck surgeon Scott M. Rickert, MD, director of the Division of Pediatric Otolaryngology at NYU Grossman School of Medicine and co-director of the Pediatric Aerodigestive Center at Hassenfeld Children’s Hospital.
Understanding the risks and obstacles, the Martins were determined to become a family of three.
About the EXIT Procedure
On August 3, 2021, at age 38, Yadi had an EXIT procedure, a high-risk, complex delivery for her and the baby.
In the mother’s womb, the fetus exchanges oxygen through the umbilical cord. “Once the umbilical cord is cut,” says Dr. Roman, “the baby will no longer receive oxygen, since they’re not able to breathe independently due to the obstructed airway.”
During the EXIT procedure, the baby’s head and shoulders are delivered via a partial cesarean birth, leaving everything below the chest within the uterus. At this point the umbilical cord and placenta remain intact, so they can continue to deliver oxygen, while pediatric surgeons work to establish an airway.
“It’s like pausing midbirth,” says Dr. Roman. “The minute this baby’s head is out, there is a 5- to 10-minute window to establish an airway, requiring full coordination and months of practice and planning.”
Because of the complex nature of the case, the Martins had a team of more than 25 providers within NYU Langone. Specialists in maternal–fetal medicine, neonatology, pediatric surgery, pediatric otolaryngology, and pediatric anesthesiology all worked together to deliver Aydin.
The EXIT delivery team featured Dr. Roman, who led the surgery and delivery of the baby in order for the airway to be established; Dr. Rickert, who worked to evaluate Aydin’s airway and complete a tracheostomy, a surgical procedure to create an opening through the neck into the trachea; and Dr. Fisher, who conducted further interventions for Aydin after birth.
“One of the biggest challenges for me prior to the birth was not fully understanding how blocked the airway was,” says Dr. Rickert. “Upon evaluation, there was no opening to the airway whatsoever. So we bypassed the blockage by placing a tracheotomy, successfully providing a quick intervention to then complete the delivery. But just because we had the airway secure and him safely breathing didn’t mean that Aydin was fully in the clear.”
CHAOS syndrome comes with accompanying challenges. Once Aydin was successfully delivered, the care team discovered more obstacles ahead.
Complex Care in the Operating Room
Aydin’s lungs were inflated because of the airway obstruction. This put pressure on his heart, affecting its ability to function properly. Moments after the EXIT, neonatologists started to resuscitate Aydin, but it was clear his heart was not recovering. Dr. Fisher made the quick decision to initiate ECMO, or extracorporeal membrane oxygenation, a treatment that takes over the work of the heart and lungs, allowing them time to heal.
“Once he was stable, we made a final discovery—Aydin had another birth defect. An anorectal malformation, meaning his anus hadn’t formed properly,” explains Dr. Fisher. “We planned for every contingency imaginable, and he still threw us some curveballs.”
Aydin was transferred to the NICU in critical condition—still on ECMO, but with an assisted airway established.
Dedicated Care in the NICU
Twenty-four hours after birth, the care team made the decision to wean Aydin off ECMO support. “Aydin’s success in the discontinuation of ECMO therapy was a huge indication his health was starting to improve,” says Dr. Fisher.
Over the next 169 days in the NICU, Aydin miraculously got stronger, overcoming various obstacles and hitting important milestones along the way.
On September 7, 2021, when he was just over a month old, Yadi and Jamaal were finally able to hold Aydin for the first time. It was a huge moment for the grateful parents. “We’re so lucky he’s alive and in our arms,” recall the Martins.
“Parents like Aydin’s unfortunately need to be separated from their babies for good reason…so we can save their child’s life. Being able to reunite them and have them hold their baby in their arms is one of best moments in our work, and it was particularly meaningful for this family, who had been through so much,” says Robert M. Angert, MD, associate professor in the Department of Pediatrics and a neonatologist at Hassenfeld Children’s Hospital. He was in the operating room when Aydin was born and was one of the many specialists that cared for him during his many days in the NICU. “Taking care of Aydin was indeed a team effort, and partnering with this family, who have such a positive outlook, made caring for him a true joy.”
“The entire NICU team were like the silver lining in this whole experience,” recall the Martins. “We left the NICU with essentially family—so many new aunts, uncles, grandparents. They were completely integral in Aydin’s success.”
Aydin had other procedures, including heart surgery to correct his congenital heart defect, performed by T.K. Susheel Kumar, MD, pediatric cardiac surgeon in the Pediatric Congenital Heart Program at Hassenfeld Children’s Hospital; and a procedure to fix his anorectal malformation, performed by Dr. Fisher, who also runs the newly established Pediatric Complex Colorectal Care Program.
On Yadi’s 39th birthday, January 19, 2022, Aydin was transferred from the NICU at Hassenfeld Children’s Hospital to the Children’s Specialized Hospital in New Brunswick, New Jersey, a rehabilitation facility that would help the Martins prepare to take Aydin home.
A Bright Future Ahead
Aydin continued to improve. He was brought home to Brooklyn for the first time six months later, celebrating his first birthday on August 3. The Martins are most looking forward to watching Aydin grow like a normal baby, now that he’s home and out of the hospital.
Aydin’s care team is optimistic about his future. “While Aydin is doing remarkably well, he has at least one more surgery necessary before he will be able to breathe completely on his own,” says Dr. Rickert. “We plan to keep monitoring Aydin’s airway and do a reconstruction in the next few years, when he’s grown a bit bigger.”
“The team at Hassenfeld Children’s Hospital is now family to us,” says Yadi. “We were in the safest place we could be for us—and for Aydin. I am forever grateful.”
Media Inquiries
Katie Ullman
Phone: 646-483-3984
kathryn.ullman@nyulangone.org