NYU School of Medicine Says Yes

Visualization tools like augmented reality bring a powerful new dimension to learning gross anatomy.
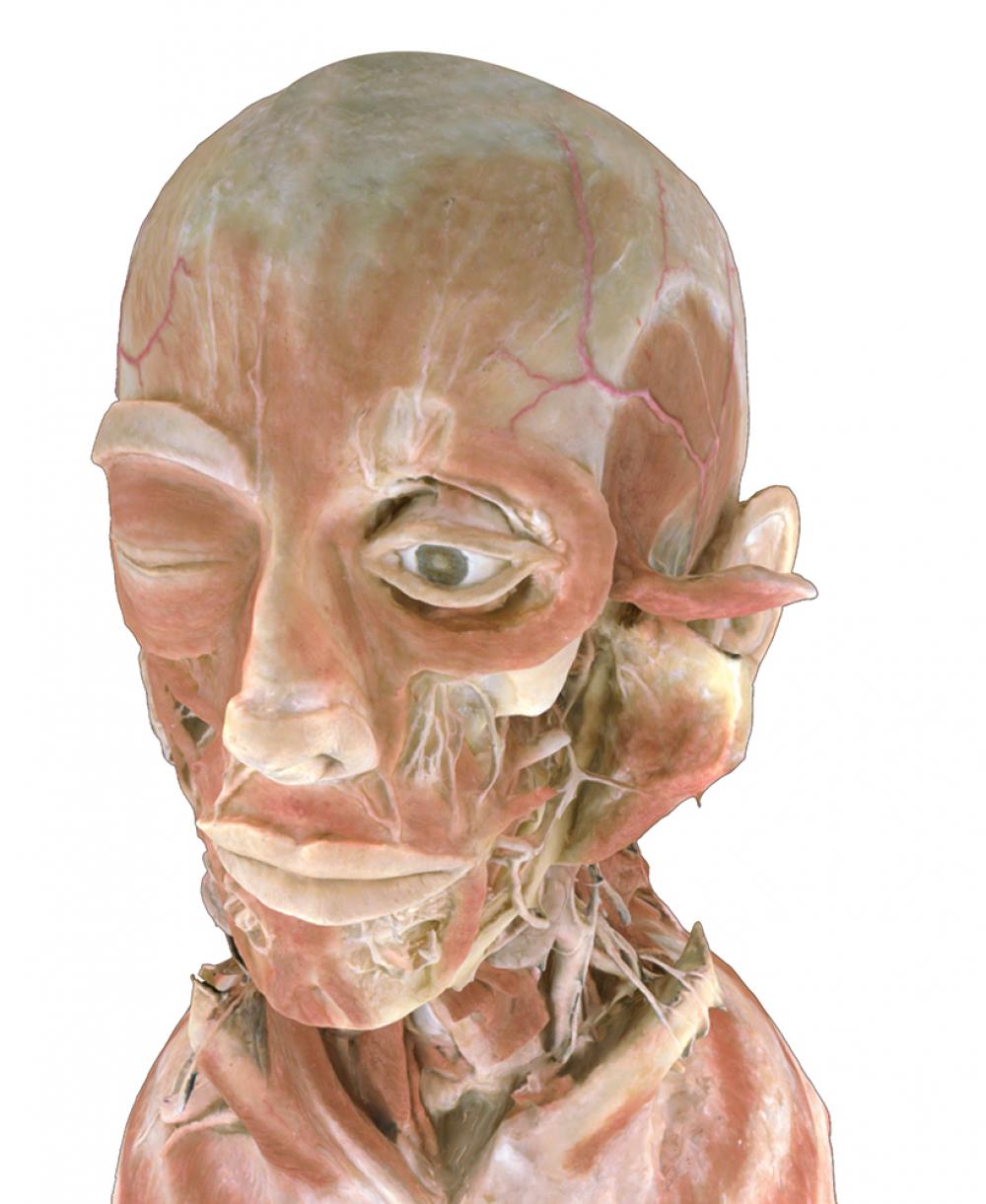
Photo: Sasha Nialla
There’s a hollow space in the human skull that’s no bigger than a hazelnut but is a major source of headache for medical students: the pterygopalatine fossa. This hidden labyrinth of canals, tucked behind the jawbone, houses a bundle of nerves and vessels supplying all of the facial structures. Studying it is a real strain on the imagination because no one can actually see this body part, at least not without destroying the skull.
“Students can sort of find it during dissection, but it doesn’t look like much after they’ve broken apart the skull to get to it,” says Victoria M. Harnik, PhD, associate dean for curriculum at NYU School of Medicine. “It’s a prime example of the limitations of cadavers.”
In the four decades that Dr. Harnik has been teaching gross anatomy, human dissection has figured prominently in her instruction. But this August, for the first time in NYU School of Medicine’s 178-year history, students will learn anatomy without it. Instead, they will rely on modern teaching aids, like virtual and augmented reality, three-dimensional cinematic renderings of CT and MRI scans, and a new collection of plastinations—human cadavers preserved with plastic resins. In a pilot run of the new curriculum last year, upper-level students found training without human dissection comparable to their experience with the cadavers, says Dr. Harnik.
While NYU School of Medicine will retain some cadavers for demonstration purposes, the inaugural anatomy module taught at the new NYU Long Island School of Medicine, which welcomed its first 24 students last month, will eliminate cadavers altogether. This historic shift is part of an institution-wide embrace of technology at NYU Langone Health, led by Robert I. Grossman, MD, the Saul J. Farber Dean and CEO of NYU Langone Health, whose vision for modernizing medicine has driven paper medical records at the institution to the point of extinction and ensured that the Helen L. and Martin S. Kimmel Pavilion, opened last summer, is now among the most digitally sophisticated inpatient facilities in the nation.
Setting aside the technical challenges of reaching the body’s many nooks and crannies without destroying them in the process, it’s often difficult to link anatomical structures to clinical problems in a body without a pulse. What’s more, cadavers are expensive to acquire and maintain. With newer digital tools, students can rotate a heart in three dimensions and observe how it behaves, say, when a valve leaks, or they can crack open a skull to see the pterygopalatine fossa, intact and in context, and then put it all back together again.
“We now have access to a wide range of rich visualization tools that represent a big part of the future of healthcare practice, not just medical education,” says Marc M. Triola, MD, associate dean for educational informatics and the founding director of NYU School of Medicine’s Institute for Innovations in Medical Education (IIME), which has partnered with the Office of Medical Education to implement the new anatomy modules.
Gregory Dorsainville, senior multimedia developer at IIME, who oversees the design, development, and implementation of augmented and virtual reality, believes the technology not only helps teach anatomy but also gives learners valuable exposure to broader trends in clinical practice. “Whether it’s planning neurosurgeries or visualizing three-dimensional radiographic studies,” Mr. Dorsainville notes, “being able to use these technologies to explore and understand the human body in new ways is a key part of the future.”
Nationwide, only a handful of other medical schools have abandoned cadavers, and the jury is still out on the educational value of virtual and augmented reality. But the goal of the reimagined teaching module, called Living Anatomy, is not simply to replace cadavers with technology, but to find the optimal way to teach anatomy. That effort enlists a team of anatomists, pathologists, and radiologists to help rethink the modules and place new emphasis on multidisciplinary integration. “Each time students see an anatomical structure, they are also shown the imaging side of it,” says radiologist Kira Melamud, MD.
“The idea is to help students learn anatomy in the context of diseases and clinical practice,” adds pathologist Amy V. Rapkiewicz, MD, director of the Integrated Anatomy course debuting at NYU Long Island School of Medicine. “What we’re really doing is making a better anatomy module that brings anatomy to life in ways that were impossible in the past.”