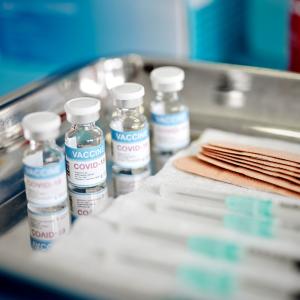
NYU Langone researchers, including infectious diseases expert Dr. Mark J. Mulligan, are among the first to enroll patients in a clinical trial of COVID-19 vaccines against the pandemic coronavirus.
Photo: NYU Langone Staff
The first U.S. patients have been dosed in a clinical trial testing whether four experimental messenger RNA (mRNA) vaccine candidates can prevent infection with the virus that causes 2019 coronavirus disease (COVID-19).
Pfizer Inc. and BioNTech SE today announced the trial’s start, with NYU Grossman School of Medicine and the University of Maryland as the first centers to enroll patients in the United States. The randomized phase 1 and 2 clinical trial will seek to enroll healthy patients to receive either one or two doses of one of the vaccines or a placebo (saline solution). The vaccines are being developed by Pfizer and BioNTech, which recently launched a similar, first-in-human trial in Germany.
Vaccine designers at BioNTech sought to determine which protein components of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) were “most noticed by” the human immune system. Successful vaccine ingredients “teach” the immune system which microbial invaders to attack upon future encounters, providing protection for a period of time, researchers say.
“We are excited to work with industry leaders to rapidly, carefully test state-of-the art vaccine candidates, with the goal of providing protection against this pandemic that has taken such a tremendous toll,” says Mark J. Mulligan, MD, director of the Division of Infectious Diseases and Immunology and the Vaccine Center at NYU Langone Health. “Vaccines have always been our most effective weapons to protect the health of the public from infectious disease threats, which is why it’s so important to study these candidates closely.”
VIDEO: Mark J. Mulligan, MD, discusses the clinical trial of experimental COVID-19 vaccines that is underway at NYU Grossman School of Medicine and other sites in the United States.
NYU Langone Health was chosen as a trial center thanks in part to the expertise of Dr. Mulligan, a leader in infectious disease research programs that have over decades yielded vaccine candidates for HIV and other viruses. NYU Langone and the other trial centers—the University of Maryland, University of Rochester, and Cincinnati Children’s Hospital—were also chosen because of their capability to rapidly launch vaccine trials, researchers say.
The study vaccines are part of the class called “mRNA vaccines” that with recent advances can quickly be computer-designed, fabricated, and scaled up into millions of doses if successful and pending regulatory approval using high-speed machines. RNA-based vaccines also by nature avert risks of infection and immune challenges that come with older vaccine types based on live, weakened versions of a virus.
New Generation of Vaccines
mRNA vaccines are based on RNA, or ribonucleic acid, a form of genetic material similar to DNA. Human cells use mRNA to translate DNA instructions into proteins, the workhorse molecules that make up cell structures. In some viruses, including the new coronavirus, RNA serves as the primary genetic material instead of DNA.
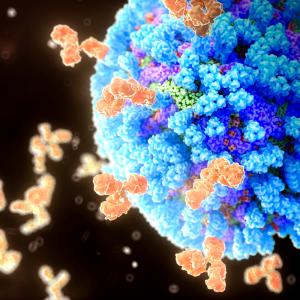
Thus, two of the study vaccines contain viral RNA encoding the “spike proteins” used by SARS-CoV-2 to attach to proteins on human cell surfaces, the first step in invading cells. Including the spikes in vaccines has the potential to make proteins required for viral survival (ability to infect) visible to the human immune system, say the study investigators. Interestingly, the specific region of the spikes that enables their attachment to cells, receptor-binding domains (RBDs), may generate antibodies even better able at disabling the virus, researchers say. For this reason, two of the study vaccines feature RBDs.
In the study, vaccine injections will deliver small segments of mRNA into the arm muscles of participants. All mRNA versions are encased in a fatty lipid particle meant to prevent their destruction by enzymes, and to let them persist long enough to enter the cytoplasm of cells in muscle and nearby lymph nodes. Once there, the spike or RBD protein is made and triggers antibody and cellular immune responses.
The research program will proceed in stages, say the investigators, with the current, initial “dose escalation phase” to gather evidence on safety, best dose, and number of doses by midsummer in 360 healthy subjects in two groups: 18 to 55 and 65 to 85 years of age. The first subjects immunized will be younger, healthy adults aged 18 to 55. Older adults will only be immunized with a vaccine candidate once testing in younger adults has provided initial evidence for safety and desired immune responses.
Media Inquiries
Greg Williams
Phone: 212-404-3500
gregory.williams@nyulangone.org