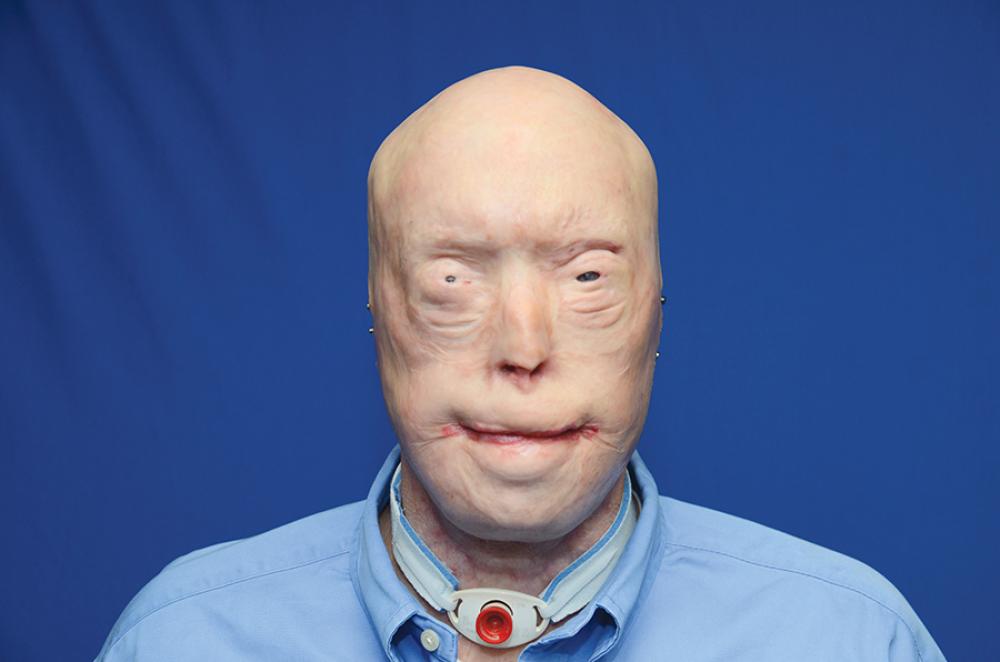
Face transplant recipient Patrick Hardison, one year after his procedure.
Photo: Ben Rollins
Before his face transplant last year at NYU Langone, Patrick Hardison made a deal with his surgeon, Eduardo D. Rodriguez, MD, DDS. “I said, ‘You do your part, and I’ll do mine,’ ” recalls Hardison. A former volunteer firefighter from Senatobia, Mississippi, he had been severely disfigured when a burning roof collapsed on his head, destroying his eyelids, lips, ears, and nose, and leaving a mass of scar tissue from the scalp down.
As the world learned, Dr. Rodriguez and his team of over 100 came through on their end, successfully completing the most extensive face transplant ever performed in just under 26 hours on August 15, 2015. “No one had ever replaced so much tissue before, including functional eyelids,” explains Dr. Rodriguez, the Helen L. Kimmel Professor of Reconstructive Surgery and chair of the Hansjörg Wyss Department of Plastic Surgery. And one year later, Hardison, for his part, is still making good on his end of the deal. “I wasn’t going to let everybody else do all this work, and then suddenly say, ‘Okay, forget it,’ ” says Hardison. “I’m not that guy.”
Hardison’s commitment to his new face has played a big role in his unusually smooth recovery. Of the 37 men and women who’ve undergone such procedures, almost all have experienced an episode of acute rejection, usually within 90 days. Hardison still hasn’t had one. Aside from a brief viral illness, he has suffered no opportunistic infections or other significant adverse effects of antirejection medications. “Patrick’s recovery has amazed us all,” says Bruce Gelb, MD, assistant professor of surgery and director of renal transplantation, who designed Hardison’s regimen of immunosuppressant medications.
Today, Hardison can perform all the ordinary functions that eluded him for more than a decade after his 2001 accident. The father of five can close his eyes, form normal facial expressions, and eat without pain. His restored ability to blink (and thus keep his eyes clean and hydrated) means he’s no longer at risk of going blind. To his delight, he can drive a car again.
There have been struggles along the way. Hardison had to learn how to swallow and talk again following the surgery, and he’s undergone revision surgeries to adjust his new eyelids, lips, and forehead. Even today, his swelling has not yet fully subsided. But compared to other face transplant patients, his progress has been remarkable.
Dr. Rodriguez attributes his success to a variety of factors, including the exhaustive testing that was done to ensure that the donor would be a favorable match. He also credits a dose of rituximab (often used in kidney transplants, but never before in a face transplant) after the surgery to reset immunological memory in Hardison’s B lymphocytes, as well as a slower-than-usual postoperative tapering of other antirejection drugs. Another new technique, transplanting portions of the donor’s facial skeleton, was used to provide better support for soft tissues, and Dr. Rodriguez theorizes that the bone may be releasing stem cells that are helping Hardison’s new face to thrive. Finally, there’s Hardison’s excellent compliance: he takes his medications faithfully, exercises regularly, and avoids alcohol and tobacco. “I do what I’m supposed to do as well as I can,” Hardison notes. “That’s what I promised Dr. Rodriguez.”
“I go about my day just like anybody else. There are no more stares, no more frightened children running away from me. I’m pretty much just a normal guy.”—Patrick Hardison
Dr. Rodriguez and his colleagues recently published their findings in a series of articles in the journal Plastic and Reconstructive Surgery. The Department of Defense, meanwhile, has awarded Dr. Rodriguez $2.5 million for further research, hoping such methods can be applied to a wide range of composite vascularized allografts.
For Hardison, however, the payoff is already apparent. “I go about my day just like anybody else,” he says, marveling at the idea. “There are no more stares, no more frightened children running away from me. I’m pretty much just a normal guy.”