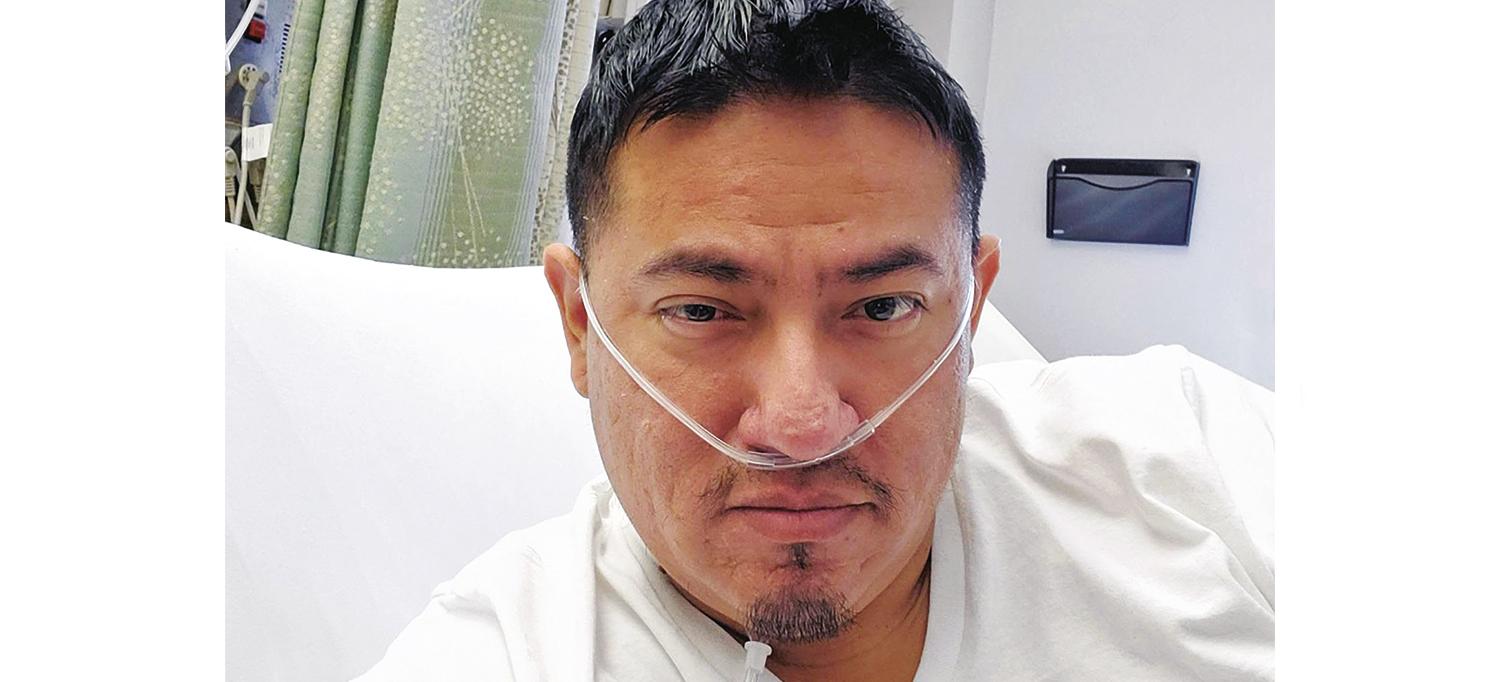
At NYU Langone Hospital—Long Island, Miguel Chamaidan, the first patient in NYU Langone Health’s system to be hospitalized for COVID-19 during the spring surge, was treated with high-flow oxygen therapy. For some patients, this noninvasive technique provides appropriate respiratory support and ensures that ventilators are available for those who can’t survive without them.
Photo courtesy of Miguel Chamaidan
On March 29, NYU Langone Health received 55 additional ventilators from New York state for patients with coronavirus disease (COVID-19) in need of mechanical respiratory support until their lungs could recover well enough to function on their own. A dire shortage of ventilators nationwide had dominated the headlines for weeks, and five days before these reinforcements arrived, Governor Andrew Cuomo projected that New York state alone would need 30,000 of the lifesaving devices.
In advance of the spring surge, NYU Langone’s leadership had deep discussions about a strategy for optimizing care for patients who require respiratory support when ventilators are in short supply. One highly controversial protocol, approved for emergency use by the State of New York, calls for splitting ventilators among patients. But the risks are steep, including potential cross-contamination and the inability to individualize the ventilator settings. “Many institutions had moved to a model where they would split ventilators or allocate them based on age, comorbidities, or other criteria,” says Robert J. Cerfolio, MD, MBA, professor of cardiothoracic surgery and chief of hospital operations. But splitting ventilators, he notes, should be the very last option because it requires nearly identical compliance from both patients’ lungs to ensure that each person receives adequate oxygenation and ventilation.
“We felt very strongly that we should not allocate or split ventilators," says Fritz François, MD, chief medical officer and patient safety officer. “We needed to explore other options.” He explains that for some patients, noninvasive techniques, such as high-flow oxygen therapy—in which the rate at which a patient receives oxygen is dramatically increased—provide appropriate respiratory support and ensure that ventilators are available for those who can’t survive without them. Moreover, he felt that prematurely enacting a policy of allocating ventilators—a decision process made by a committee far removed from bedside care—would go counter to one of NYU Langone’s bedrock principles of clinical care. “We believe that the clinician who is caring for a critically ill patient is best able to make an assessment and decision. We let doctors be doctors.”
NYU Langone’s thoughtful approach to ventilator use is well aligned with the lessons intensivists have learned as they’ve treated more and more patients with COVID-19. “Over time, we’ve recognized that a ventilator isn’t the best option for all of these patients,” explains Mark E. Nunnally, MD, director of adult critical care services. “Instead of intubating patients early on, we manage them with high-flow oxygen therapies, providing progressive support until they are unable to maintain a satisfactory oxygen level.”
Even at the peak of the spring surge, only 58 percent of NYU Langone’s ventilators were in use. “The fear of not having enough did keep me awake at night,” says Dr. Nunnally. “But we were able to stay ahead, even in the darkest moments. And for some patients, the brightest moment came when they recovered so well that they could be weaned off the ventilator.”

