Photo: stockdevil/Getty
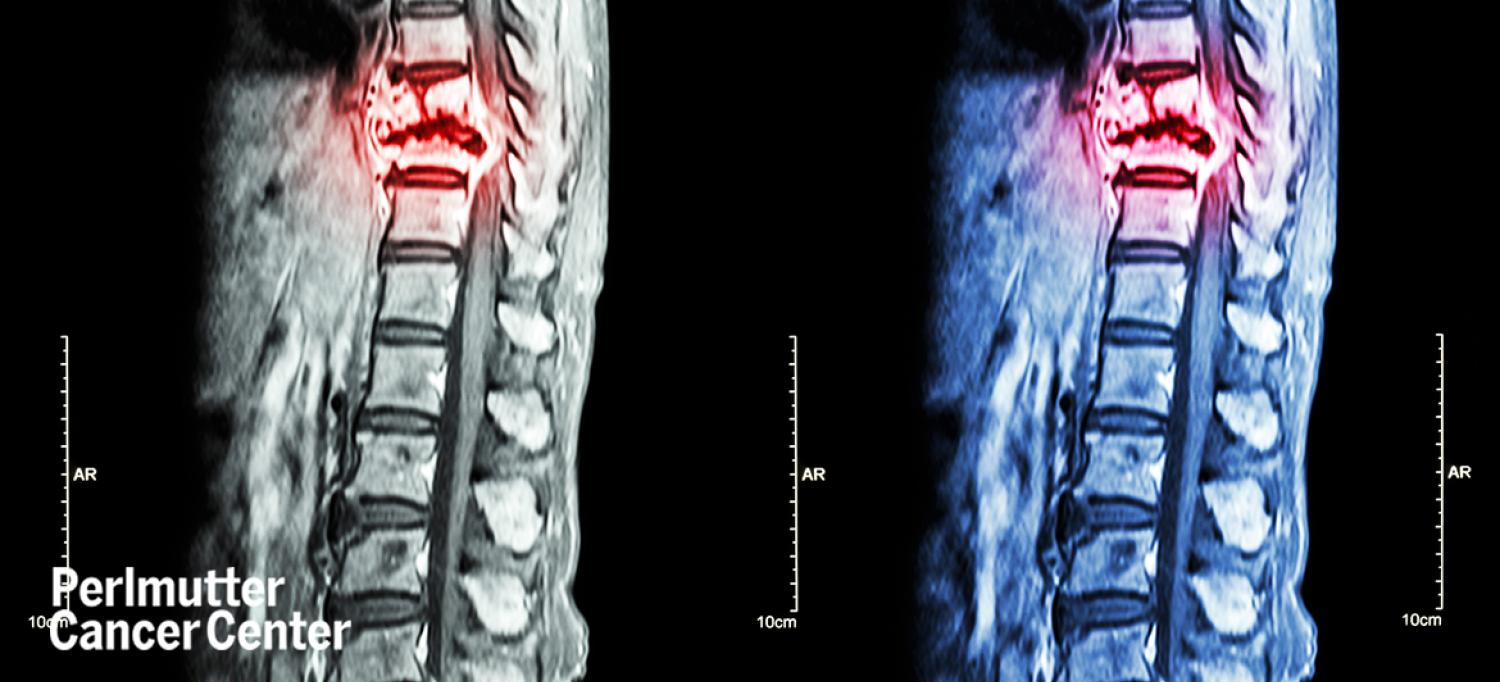
A patient at NYU Langone Health’s Perlmutter Cancer Center needed radiation treatment for cancer that had metastasized to the spine. But with a full-time job and other commitments to work around, the typical eight-day timeline for receiving treatment—which includes multiple appointments with a variety of specialists at the cancer center—wasn’t going to work.
To help this patient, Thomas B. Daniels, MD, a clinical associate professor and associate medical director of the Department of Radiation Oncology at NYU Grossman School of Medicine, led a multidisciplinary team that implemented Perlmutter Cancer Center’s first same-day spinal radiosurgery.
The procedure consolidated the usual eight days of treatment planning and delivery of radiosurgery into a single day, providing this patient with prompt relief of painful symptoms and an improved outcome.
“The introduction of same-day spine radiosurgery is poised to revolutionize patient care and transform the landscape of spinal metastasis treatment,” said Alec Kimmelman, MD, PhD, the Anita Steckler and Joseph Steckler Chair of the Department of Radiation Oncology at NYU Langone, where he is also a professor. “This breakthrough paradigm allows us to streamline the treatment process, reducing the burden on patients and optimizing their overall experience.”
Spinal radiosurgery requires multiple steps and involves a number of specialists. First, a CT scan is taken with the patient in a custom-made immobilization device, which helps them stay in the same position for radiation treatment. The CT scan is then synced with the patient’s MRI scan, which radiation oncologists examine slice by slice to define the areas they need to treat. A dosimetrist develops a radiation plan based on the analysis of the MRI, and a physicist provides quality assurance.
Dr. Daniels said same-day spinal radiosurgery is currently appropriate for patients with cancers that have only a few, generally small, metastases. This type of cancer is described as oligometastatic.
“The patient we treated had one area of progression on imaging, so we wanted to be aggressive with the treatment,” Dr. Daniels said. “The patient was able to come in the morning and receive treatment in the afternoon. This was ‘one-stop shopping’ as opposed to multiple outpatient appointments and delays.”
There were a couple of factors that led the team to move forward with an accelerated treatment schedule. Given that the patient had a full-time job, the same-day spinal radiosurgery was particularly convenient, Dr. Daniels said. And with only one area of disease progression and an otherwise well-managed disease, the patient was an ideal candidate for the procedure, which involved a high dose of radiation.
“Traditionally patients with stage IV disease were considered terminal and treated with chemotherapy,” Dr. Daniels said. “But now, with better systemic and local therapy options, we are taking patients who are technically stage IV and treating them with curative intent.”
In addition to Dr. Daniels, about 30 people were involved in the planning and execution of the same-day radiosurgery. Physicists played a key role in the planning of the procedure, and Dr. Kimmelman credited Martha J. Malin, PhD, an assistant professor in the Department of Radiation Oncology and principal project physicist, for her expertise in a technology that uses imaging techniques to monitor the position of the tumor and surrounding tissues in real time.
“I want to give Dr. Malin particular recognition for being a true driver of this program, spending countless hours on the radiosurgery and same-day programs,” Dr. Kimmelman said. “Without her amazing abilities as a physicist, none of this would be possible.”