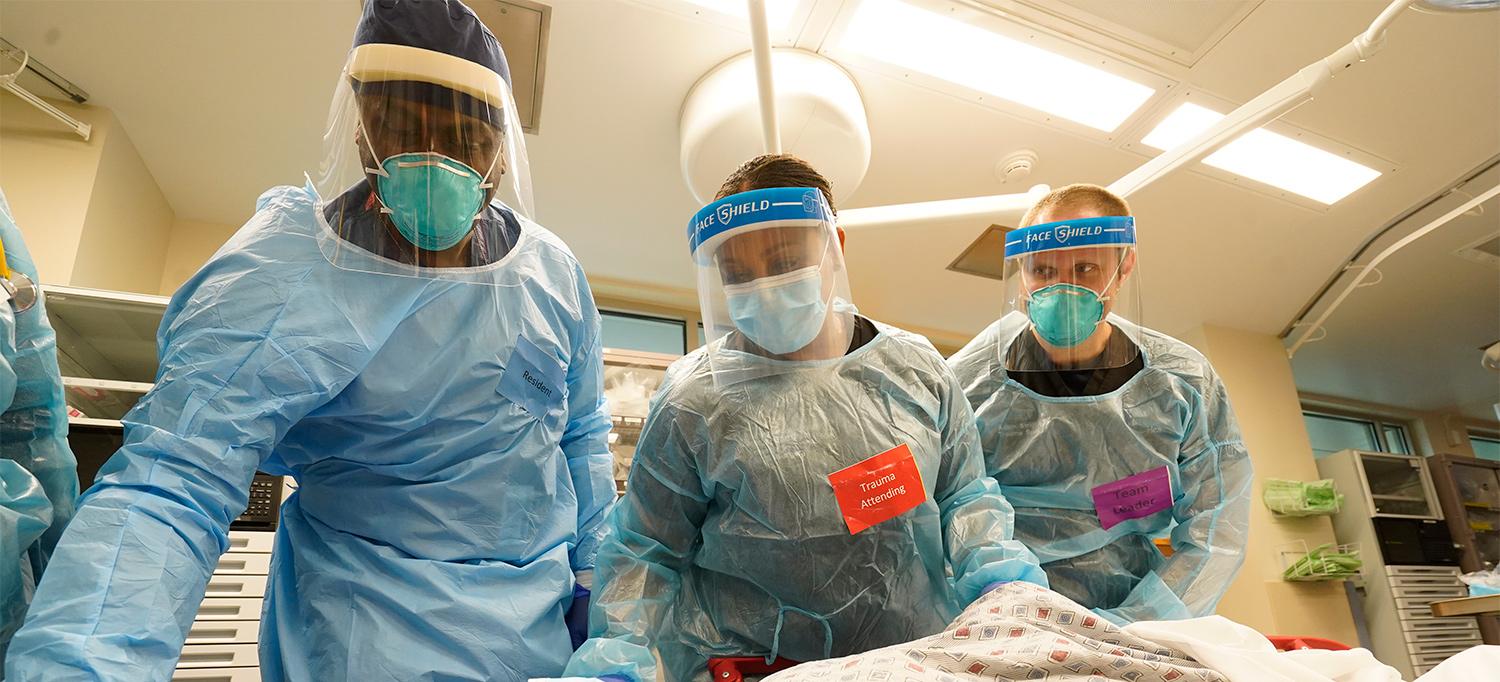
At NYU Langone Hospital—Long Island’s Trauma Center, respiratory therapist Jeff Espert and acute care and trauma surgeons Dr. D’Andrea Joseph and Dr. Adam Stright demonstrate emergency care procedures on a mock patient.
Photo: Gregory Shemitz
At 3:00AM on April 4, Easter Sunday, a 28-year-old resident of Elmhurst, Queens, was in the passenger seat of a car that raced along Jericho Turnpike in Mineola, Long Island. In a split second, the car lost control and collided with two other vehicles, crashing into a storefront. Upon impact, the car split in two, with the back end engulfed in flames and the front overturned into a brick wall. The woman and her friend who was driving the car were hurled through the windshield.
The driver, thrown the length of a football field, did not survive. The woman was pinned between a section of the chassis and the wall. Emergency medical service (EMS) technicians worked quickly to extricate her, alerting the Emergency Department at NYU Langone Hospital—Long Island, just one mile away, of the imminent arrival.
The team at the hospital’s Level 1 Trauma Center, 1 of 3 in Nassau County, cares for some 2,200 accident victims each year. More than 20 percent of the blunt or penetrating injuries are severe enough to threaten life or limb. The woman’s dire condition, however, would test the limits of the team’s prowess. Her injuries included collapsed lungs, multiple fractured ribs, a broken right thighbone, several spinal fractures, extensive lacerations to both lobes of her liver, and a fist-sized puncture in her lower back. Acute care and trauma surgeon Adam E. Stright, MD, assistant professor in the Department of Surgery at NYU Long Island School of Medicine, was on call that night and led the effort to resuscitate the woman. He described her condition as nearly “unsurvivable.”
At the crash scene, the woman was found unconscious. “Her heart had stopped beating,” explains Dr. Stright. When she was wheeled into the trauma bay, the team continued the cardiopulmonary resuscitation (CPR) begun by EMS. Laura M. Velcu, MD, another acute care and trauma surgeon, helped stabilize the patient for transfer to the operating room (OR). Among other interventions, the team inserted tubes to decompress her chest and performed a transfusion to stem her massive blood loss. “It took more than 30 minutes to finally get her pulse back,” says Dr. Stright. When a patient’s heart has stopped beating for more than 20 minutes, the risk of irreparable brain damage or death skyrockets. “She is really weak,” Dr. Stright told a relative. “She might not make it through the night.”
There’s no set cutoff point for when to discontinue resuscitation efforts, he explains. In this patient’s case, he kept going because he found considerable cause for hope. She was young and otherwise healthy. Moreover, the team did not identify a major brain injury, which would cause neurologic deficits that preclude a meaningful recovery. Dr. Stright also noticed that the patient was coughing, evidence that her brain was still functioning. “These sustained signs of life guide our clinical judgment and tell us that what we’re doing is working,” he says. “Our singular mission is to get the patient through the worst day of their life so that they can come out on the other side.”
The trauma team packed the wound in the woman’s lower back to control blood loss, but they couldn’t be sure whether her state of shock was due to internal bleeding. When an abdominal ultrasound indicated the presence of blood, explains Dr. Stright, “we knew that the only way to save her was to get her to the operating room to perform exploratory surgery.”
En route to the OR, the anesthesiologist reported that the patient’s blood pressure had dropped so low that it was undetectable. Dr. Stright performed CPR again, this time for 15 minutes. “I could feel a pulse in her carotid artery,” he says, “so I decided to proceed with the surgery, delivering blood throughout the operation.” Dr. Stright repaired a severe injury to the patient’s liver, which stopped the internal bleeding, but because her abdomen was too swollen to suture, closure of the muscle layer was later performed by acute care and trauma surgeon Gerard A. Baltazar, DO.
After Dr. Stright’s surgery, the patient’s condition stabilized, but persistent bleeding from the puncture in her lower back caused her blood pressure to drop. Vascular interventional radiologist Man Hon, MD, identified the ruptured blood vessel and blocked it off to stop the bleeding.
The patient required several weeks of intensive care to recover from her blood loss, and multiple surgeries to repair fractures to her spine and leg, but she was finally on the road to recovery. On the woman’s birthday, she had the last of her surgeries, a skin graft performed by acute care and trauma surgeon D’Andrea K. Joseph, MD. She was discharged from the hospital one week later. As chief of the Division of Trauma and Acute Care Surgery at NYU Long Island School of Medicine, Dr. Joseph oversees the care of complex cases. “The patient’s prognosis is excellent,” says Dr. Joseph. “She has a bit of weakness in her right leg, but with physical therapy, she should be able to overcome this.”
The remarkable comeback of the patient underscores the breadth and depth of the Level 1 Trauma Center’s expertise. “We do this work knowing that if the patient gets to us in time, we can intervene and save their life,” says Dr. Joseph, who notes that a multidisciplinary array of specialists is always on call. “I lead the team with that attitude.”
Dr. Joseph, who joined NYU Langone in 2017, explains that she came to NYU Langone Hospital—Long Island, in large part, because she felt a kinship with Collin E. Brathwaite, MD, chair of the hospital’s Department of Surgery. Like Dr. Joseph, Dr. Brathwaite trained at the renowned R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center. The first hospital dedicated exclusively to trauma care, it provided a model for expediting the arrival of patients through a dedicated trauma bay that is separate from the emergency department.
The patient, now a premed student, plans to emulate her doctors and become a trauma surgeon. “Dr. Stright and his team never gave up on me,” she says. “They saved my life. I’m never going to forget what they did for me.”

