Research led by vascular neurologist Dr. Shadi Yaghi aims to better understand the origins of stroke so doctors can personalize prevention and treatment approaches for each patient.
Photo: NYU Langone Staff
At NYU Langone’s Comprehensive Stroke Center, researchers are engaged in groundbreaking investigations across the spectrum of stroke care, deepening their understanding of the root causes, pathologies, and mechanisms to redefine quality in stroke care and prevention.
Uncovering Clues for Stroke Risk Stratification
A central body of research, led by Shadi Yaghi, MD, assistant professor in the Department of Neurology, is elucidating stroke risk by revealing biomarkers associated with initial or subsequent strokes. “Although we’ve advanced the treatment of known risk factors such as hypertension, diabetes, and hyperlipidemia, stroke remains a leading cause of morbidity and mortality,” notes Dr. Yaghi. “Our research focuses on understanding the origins of stroke at a deeper, more nuanced level in order to better target prevention and treatment approaches to each patient.”
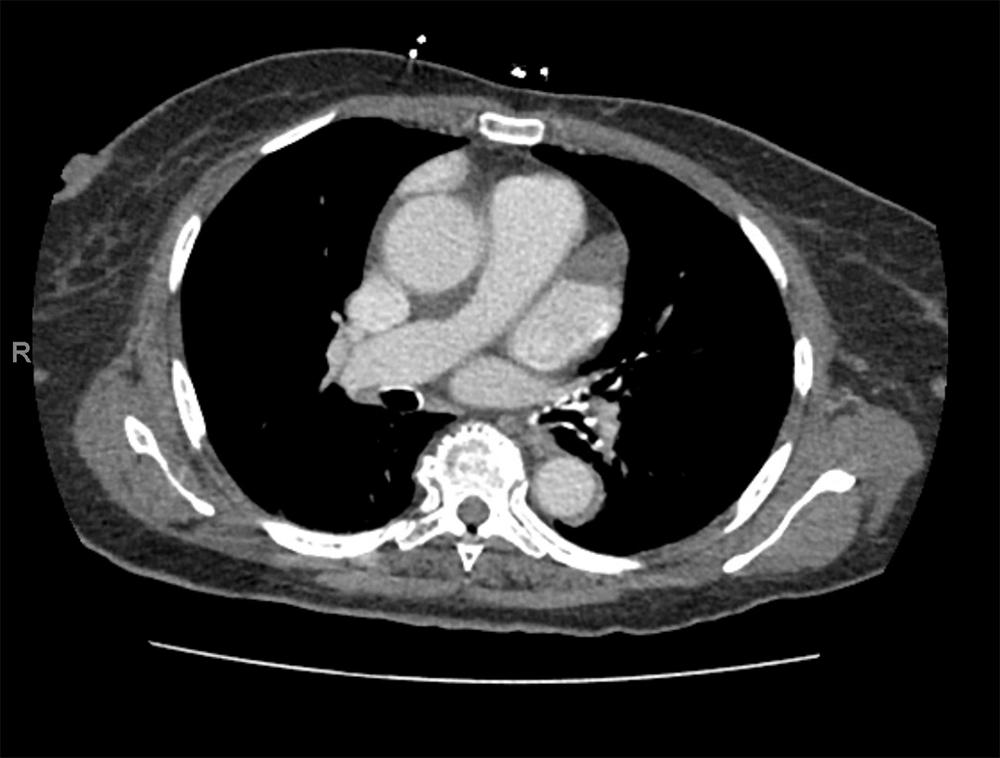
One line of research is applying advanced imaging to stratify risk in patients who have experienced a previous stroke. The research, funded by the American Heart Association and published in 2018 in the Journal of Stroke and Cerebrovascular Diseases and in 2019 in the Journal of Cardiovascular Computed Tomography, uses contrast-enhanced CT scans to examine the left atrial appendage’s structure, function, and propensity to clot. This chamber is the most common site of heart-related clots and is extremely difficult to visualize using a traditional echocardiogram.
“The gold standard for studying this chamber, a transesophageal echocardiogram, is invasive and costly,” explains Dr. Yaghi. “But the commonly used noninvasive echocardiogram just does not give us a good view of this chamber, where clots form in the heart.” The chest CT scan can provide thinly sliced views of the chamber’s morphology and volume as well as the presence of clots. Dr. Yaghi points to recent clinical cases where his use of the scans identified clots unseen by a traditional chest echocardiogram, revealing both risk and opportunity for intervention in those patients. Ultimately, he hopes to utilize this novel imaging approach to identify at-risk patients and study the potential benefit of anticoagulant therapy to prevent recurrent stroke.
In related research, Dr. Yaghi is examining biomarkers through blood tests, electrocardiograms (EKGs), and CT scans to identify chamber dysfunction that could lead to further strokes in patients who have had a stroke of unknown cause. “Prior studies of aspirin versus novel anticoagulants have failed because stroke of unknown cause is actually a big wastebasket of possible etiologies,” explains Dr. Yaghi. “Our goal is to test anticoagulation therapy in just those patients with stroke of unknown cause—and a marker of this chamber dysfunction—who might truly benefit.”
Personalizing Stent Treatment to Prevent Secondary Strokes
A quarter of documented stroke cases are recurrent, and in patients with intracranial atherosclerosis, the risk of stroke is 25 to 30 percent within 2 years, even despite aggressive medical treatment. Research by Dr. Yaghi hypothesizes that stenting may more effectively reduce recurrence risk compared with medical treatment in patients where intracranial narrowing and decreased blood flow are demonstrated first.
“Prior research, such as the SAMMPRIS trial, was halted because it targeted all patients with arterial stenting, without consideration of individual risk and benefit—and stenting is always likely to harm a subsection of patients,” notes Dr. Yaghi. “My research shows the importance of first understanding each stroke’s specific underlying mechanisms when developing a prevention approach.”
Dr. Yaghi is submitting a grant application to the National Institutes of Health (NIH) to conduct a large multicenter study to accurately identify the subpopulation of patients with intracranial atherosclerosis that are likely to fail medical treatment. It is with these patients that the safety and efficacy of stenting would be tested. “If we are able to confirm that stenting patients whose blood flow is diminished reduces their risk, it will become a new standard of care,” adds Dr. Yaghi.
Quantifying Stroke Rehabilitation by Defining Dosage
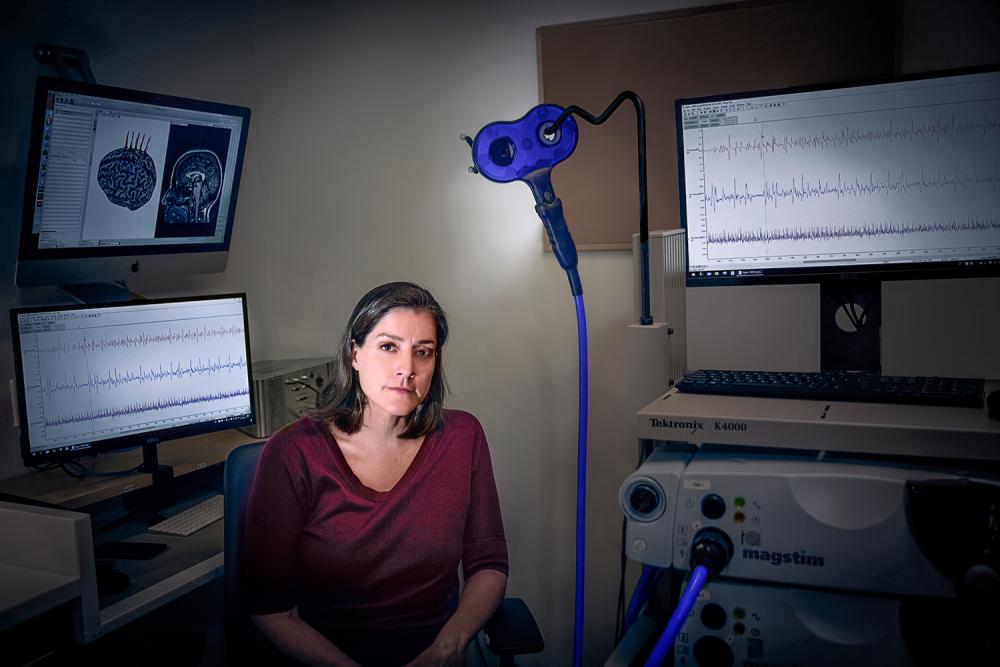
Separate NIH-funded center research is aimed at enhancing motor recovery following stroke. One study, led by Heidi Schambra, MD, assistant professor in the Departments of Neurology and Rehabilitation Medicine, will elucidate the role of the brain’s motor pathways in facilitating post-stroke recovery. Using transcranial magnetic stimulation and structural MRI, Dr. Schambra’s team is investigating how a primordial pathway, the corticoreticulospinal tract (CReST), may facilitate motor recovery as an alternative descending motor pathway when the corticospinal tract is damaged by stroke. The team expects to reveal associations between changes in strength, motor control, motor synergies, and changes to CReST. “The idea is that this pathway could be targeted with interventions such as brain stimulation to accelerate motor recovery and reduce disability,” notes Dr. Schambra.
Another ongoing study is aimed at quantifying rehabilitation dosing to better align dosing with motor recovery targets. Although animal studies have demonstrated robust upper extremity motor recovery with early, high doses of functional training following stroke, the optimal dose remains undiscovered in humans. Dr. Schambra and colleagues are developing a tool integrating wearable sensors that will measure both the number of functional movements during rehabilitation and the motor response to interventions. Machine learning algorithms developed with the NYU Center for Data Science quantify functional movements in typical rehabilitation activities that add up to a dose.
“The challenge in stroke rehabilitation is that we use a ‘black box’ approach, without consistency across therapists and institutions, or understanding of what constitutes an aggressive intervention,” notes Dr. Schambra. “We want to build scientific rigor into rehabilitation research with the precision of medication dosing, so we can give patients the intervention level known to be effective.”
A Focus on Prevention and Outcomes
Across center research, a shared focus leads the field of stroke prevention and care toward individualized methods that can deliver better outcomes. “We’re using modalities that aren’t routinely used in innovative ways to try to understand the true cause of the stroke, and focus only on targeted treatment rather than the shotgun, one-treatment-for-all approach,” notes Dr. Yaghi.