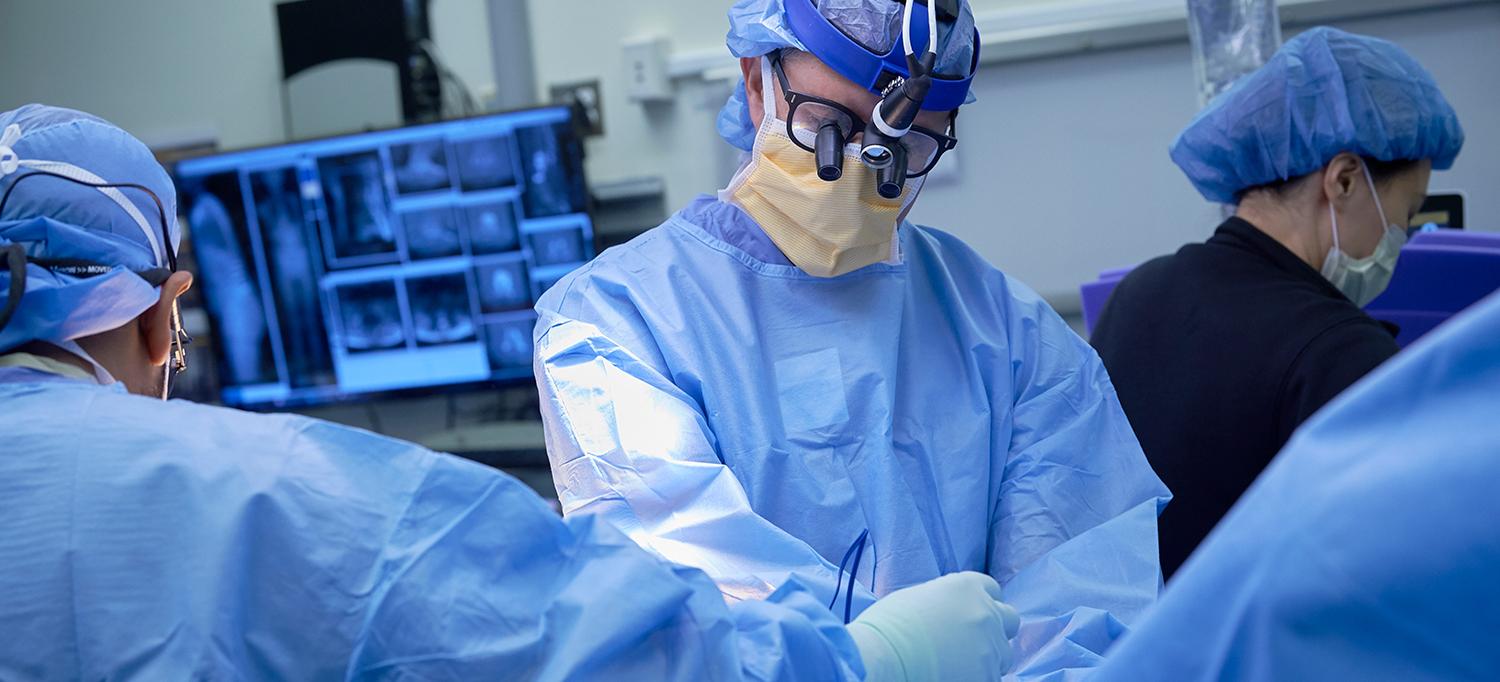
NYU Langone researchers, including orthopedic surgeon Dr. Themistocles Protopsaltis, find single-position surgery for spinal fusion is more successful than the traditional method.
Photo: Juliana Thomas
A novel approach to spinal fusion surgery results in a reduction of blood loss during surgery and less ileus, or intestinal blockage, postoperatively, as well as reduced operative times and hospital stays, according to a new study from researchers at NYU Langone Health published in The Spine Journal online November 13.
Spinal fusion, a surgery which connects two or more vertebrae in the spine to treat degenerative or deformity-related spinal conditions such as spinal stenosis, scoliosis, and spondylolisthesis, has traditionally been performed using a technique that involves repositioning the patient, or “flipping” them, midway through surgery from their back or side, to their stomach.
This new technique, called single-position anterior–posterior lumbar fusion surgery (SPLS) allows surgeons to complete the entire operation while the patient is laying on their side. This enables the surgical team to approach the spine through both the front and back—which leads to a higher fusion rate—while minimizing the amount of time needed for surgery, and allowing more rapid recovery.
“This practice-changing technique is not only just as safe and effective as the alternatives, it actually has benefits over and above the traditional method,” says lead author, Aaron J. Buckland, MD, associate professor in the Department of Orthopedic Surgery at NYU Langone. “With the improved operative efficiencies of single-position surgery, we are performing less invasive procedures, producing better outcomes, and improving safety.”
Researchers reviewed perioperative and 90-day outcomes of patients undergoing spinal fusion between May 2012 and June 2019 via a collaboration between NYU Langone Health in New York City and Atlantic Neurosurgical and Spine Specialists in North Carolina. Of the 397 procedures, 153 were classified as a “flip” procedure—meaning the patient was repositioned at least once—and 244 as an SPLS procedure.
Surgeons at NYU Langone’s Spine Center found that SPLS significantly reduced the operating time by over 3 hours, from an average time of 306 minutes to 103 minutes. An associated reduction in blood loss during the operation was also noted, as well as a decreased intraoperative radiation dosage. The length of hospital stay for patients who received the single-position technique was reduced by two days, with an average of approximately four days for patients receiving the “flip” procedure compared to fewer than two days for the SPLS patients.
The SPLS group saw lower rates of postoperative intestinal blockage, or ileus. The researchers hypothesize this is due to the reduction in time under anesthesia, more minimally invasive abdominal incisions, reduced pain medication requirement, more rapid mobilization, and the fact that patients are not laying face down during surgery. Other complications that may be reduced with the novel technique include deep surgical site infection, pressure areas, peripheral nerve injuries, and difficulties in airway access.
According to Themistocles Protopsaltis, MD, associate professor in the Departments of Orthopedic Surgery and Neurosurgery and chief of the Division of Spine Surgery at NYU Langone, and co-author of the study, “This research exemplifies the mission of our spinal surgery division to bring cutting-edge techniques to patients while improving clinical outcomes.”
Researchers of this retrospective review are opening a prospective multicenter study to evaluate SLPS against minimally invasive posterior fusion, and to further validate its efficacy.
In addition to Drs. Buckland and Dr. Protopsaltis, other NYU Langone researchers are Kimberly Ashayeri, MD, and Leon K. Eisen, MD. Coauthors from Atlantic Neurosurgical and Spine Specialists include J. Alex Thomas, MD, and Mark Medley, MD.
Media Inquiries
Annie Harris
Phone: 212-404-3588
annie.harris@nyulangone.org

