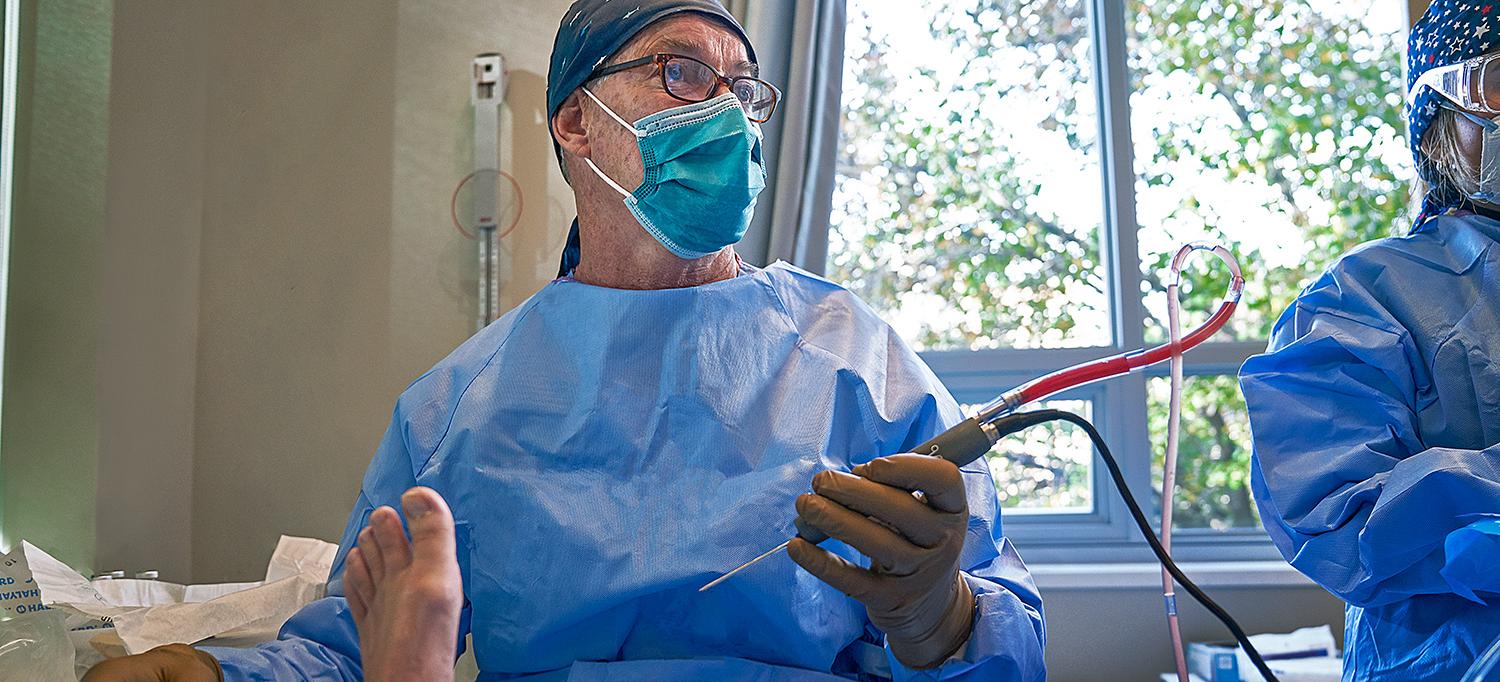
Orthopedic surgeon Dr. John G. Kennedy has pioneered an innovative, in-office visualization approach that is improving outcomes for patients with foot and ankle conditions.
Photo: NYU Langone Staff
A novel, in-office visualization approach is transforming outcomes by combining enhanced diagnostic capabilities with immediate, minimally invasive treatment for foot and ankle conditions. NYU Langone Health specialists—who pioneered the system’s use and have now performed it in the most cases worldwide—are working to extend the frontier of its applications throughout the intricate foot and ankle anatomy.
With Real-Time Insights, Enhanced Surgical Decision-Making
The nano-instrumentation technique applies a leading-edge visualization system combining imaging sensors, LED light, and image management to perform minimally invasive arthroscopy and guide injections in tight joint spaces that have previously been difficult to visualize. The needle-sized, 1.9-mm chip-on-the-tip NanoScope™ system enables diagnosis of arthritis and cartilage injuries as well as arthroscopic treatments of the foot and ankle, with local anesthesia in the physician’s office.
Pioneered at NYU Langone by John G. Kennedy, MD, chief of the Division of Foot and Ankle Surgery and professor in the Department of Orthopedic Surgery, the nano-instrumentation approach was first used to remove a patient’s bone spurs and scar tissue from a prior cartilage restoration surgery. Its benefits—the concurrent evaluation of the surgical area and immediate, targeted treatment—were apparent to the patient, who walked out of the office within 15 minutes.
“Suddenly we have the ability, outside of the operating room, to see inside joints, tendon sheaths—anywhere within the body—with clarity equivalent to or better than standard arthroscopy,” notes Dr. Kennedy.
“Patients’ understanding of their pathology can predict outcomes, and now I can show my patients what is happening—problem and solution—in real time. It’s the most interactive patients can get in their healthcare and recovery.”—John G. Kennedy, MD
Awake patients become real-time participants in their procedure and treatment. “Patients’ understanding of their pathology can predict outcomes, and now I can show my patients what is happening—problem and solution—in real time,” adds Dr. Kennedy. “It’s the most interactive patients can get in their healthcare and recovery.”
Although Dr. Kennedy has used the technique in patients of all ages, he notes that it’s most effective in mild to moderate pathologies in a younger patient population, and those patients are selected carefully. “This doesn’t displace sophisticated imaging or replace the need for larger surgeries for treatments, like implants, that can’t fit in a 2-millimeter portal,” Dr. Kennedy notes. “But I think we are heading toward a time when visiting an orthopedic surgeon will be more like visiting your dentist—you’ll go in for a small procedure and expect to leave on the same day.”
Faster Mobility Tied to Shorter Recovery
The real-time view improves visualization and understanding for both patient and physician. A patient may not comprehend why an injury causes pain during exercise, but seeing the scars and bone spurs on the ankle joint elucidates the problem. At the same time, the nano-instrumentation provides diagnostic specificity superior to that of MRI, enabling the surgeon to treat the problem immediately.
“One patient had had several MRIs with different providers, and no one could identify the source of her pain at the top of her ankle joint,” says Dr. Kennedy. “As soon as we put the camera in, we saw a loose piece of bone floating around; we took it out, and she was instantly better.”
The detailed look inside the joints has also enabled Dr. Kennedy and his team to reach—and treat—smaller areas of the anatomy. Conditions such as arthritis in the first metatarsophalangeal joint, for example, have become treatable, rather than career limiting, for athletes.
For the broader patient population, the nano-instrumentation approach has altered the course of recovery by nearly eliminating the immobilization that accompanies open surgeries due to soft tissue trauma around the target pathology. The new technique focuses recovery on the primary injury and enables immediate mobilization—critical in cartilage injuries that heal through motion.
The difference is evident in a registry of patient-reported outcome scores Dr. Kennedy created to measure overall patient satisfaction, based on factors such as mobilization and pain. In an early retrospective cohort analysis of 31 patients treated with nano-instrumentation for anteromedial impingement, known commonly as footballer’s ankle, patients demonstrated significant pain reduction and a low complication rate. Additionally, the approach was associated with excellent patient-reported outcomes and high rates of return to work and sport, with patients indicating that their involvement in the awake procedure helped them better understand their injury and recover more quickly.
Reaching Beyond the Surgical Status Quo
Dr. Kennedy and his team continue to push the boundaries of the procedure’s application to bring its benefits to more patients, and are cataloging the wide range of pathologies that may benefit, from tendon debridement to biologic augmentation of joints. The team recently achieved a plantar-plate repair with nano-instrumentation in the second toe, the world’s first recorded procedure in that area.
The technique is particularly promising in cartilage injuries, which commonly occur following minor injuries such as ankle sprains but may not present symptoms until arthritis establishes years later. Such osteochondral injuries can now be addressed in-office, where the nano-instrumentation identifies chondral defect and the patient is treated with platelet-rich plasma, significantly simplifying surgery and recovery time.
For athletes and dancers, the approach can mean the difference between returning to their full performance—or not. “Previously, we’d ask patients why they never got back to their previous levels, and they’d tell us they were overly afraid of reinjury,” Dr. Kennedy notes. “Now they can see for themselves that their injury is resolved and the joint is fine.”
The pioneering application of the technique is an example of the drive toward more sophisticated diagnostics and minimally invasive approaches to improve recovery with fewer surgical complications across orthopedic conditions, adds Dr. Kennedy. “Here, striving to be better, by doing things differently from how they were done last year or in prior years, is not only encouraged—it’s an institutional imperative,” he says. “Thanks to that culture, we’re now collaborating with surgeons around the world to help advance this approach.”
Disclosure: John G. Kennedy, MD, is a paid educational consultant to Arthrex, the company that produces the NanoScope™; he receives no financial benefit from the company’s products.

