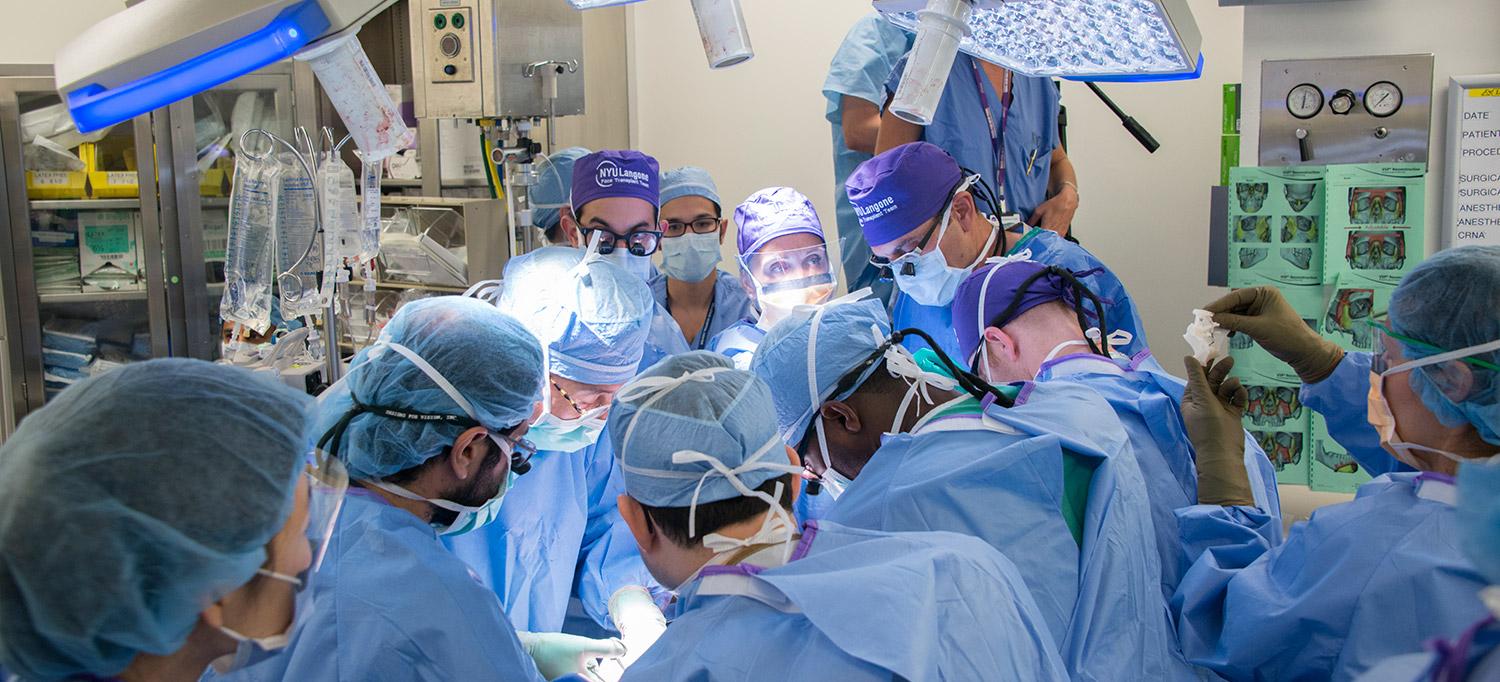
NYU Langone's surgical team successfully completed the most extensive face transplant ever performed in just under 26 hours.
PHOTO: NYU Langone Staff
At 7:00PM on August 14, 2015, surgeons lifted the skin from Patrick Hardison’s head as if pulling off a ski mask, exposing the underlying bone, muscles, ligaments, and blood vessels. With an electric saw, Eduardo D. Rodriguez, MD, DDS, removed the patient’s nasal and chin bones. The only features that remained recognizable were Hardison’s bright blue irises, staring out from naked eyeballs. “That’s when it became clear that there was no turning back,” recalls Leslie Bernstein, administrative director of NYU Langone’s Hansjörg Wyss Department of Plastic Surgery and administrator of the Face Transplant Program. Watching from across the operating room, she remembered her long talks with Hardison, at the hospital and on a visit to his hometown, Senatobia, Mississippi.
The moment came approximately 12 hours after the start of the surgery—the most extensive face transplant ever performed—and 14 years after the catastrophe that upended Hardison’s life. The volunteer fireman ran into a burning house in September 2001, searching for a woman mistakenly believed to be trapped inside. When the ceiling collapsed, he managed to escape through a window, but his head and upper body were already on fire. Hardison was still in a medically induced coma when the 9/11 attacks occurred the following week. He lost his eyelids, ears, lips, and most of his nose, and was left with a mass of scar tissue from his scalp to his chest. Despite 71 reconstructive procedures, he remained unable to form normal facial expressions, to eat or laugh without pain, or to go out in public without attracting stares. He couldn’t blink or close his eyes. Although surgeons had sutured together flaps of skin to protect his vision, he was at risk of slowly going blind.
Now, the 41-year-old father of five lay anesthetized and utterly vulnerable, awaiting a new face from a young man who’d been fatally injured two days earlier. If all went well, Hardison would regain much of what had been taken from him. If things went badly, the likely scenarios were either death or a disfigurement more severe than before.
Dr. Rodriguez, the Helen L. Kimmel Professor of Reconstructive Plastic Surgery, chair of the Hansjörg Wyss Department of Plastic Surgery, and one of the leading surgeons in his field, had spent more than a year preparing the clinicians in this room—along with dozens of others—for the groundbreaking operation. Yet even he had put the odds of success at just 50-50.
Few other surgical procedures are as medically daunting as a face transplant, and few raise as many complex ethical, philosophical, and psychological issues. “It’s at the far end of what we call the vascularized composite allografts,” observes Arthur Caplan, PhD, the Drs. William F. and Virginia Connolly Mitty Professor of Bioethics. “You’re transplanting skin, nerves, muscles, blood vessels, and other tissues all at once. The new face has to feel, taste, smell, communicate verbally and visually, and fit certain aesthetic criteria. And unlike a heart or liver, whose function is basically mechanical, a face is central to a person’s identity. Emotionally, it stands alone.”
Wanting a new face is generally not a matter of life and death. It can, however, profoundly improve a patient’s quality of life, complicating the risk-benefit calculations that must be made before any major surgery—especially a transplant, which requires the patient to take immunosuppressant medications indefinitely to prevent rejection.
The expense is another factor. A procedure that can cost nearly $1 million, including pre- and postoperative care, cannot be undertaken lightly, but the potential gains for other patients must also be considered. Although face transplantation is still in its infancy, it has already spawned technical innovations that may prove useful elsewhere in plastic surgery, transplant medicine, regenerative medicine, and beyond. The possible payoffs have attracted growing interest from some of the world’s leading academic medical centers, as well as the U.S. Department of Defense. The logistical challenges, meanwhile, have kept the pace of research slow.
The first face transplant was performed in 2005, on a French woman who’d been mauled by a dog; surgeons in Paris successfully replaced her nose, cheeks, lips, and chin. Since then, there have been 37 such procedures, but only a dozen have encompassed an entire face. Hardison’s would be the first to involve the scalp, as well, and to include functional eyelids. (In other cases, the recipients were blind, with no need to blink, or skin was simply grafted to existing eyelid muscles.) “No one had ever replaced this quantity of tissue before,” says Dr. Rodriguez. “There was no medical experience to show it was possible.”
Dr. Rodriguez was determined to prove it could be done. The son of Cuban immigrants, he’d initially set out to become a dentist (he even graduated from NYU College of Dentistry) but found his vocation after a mentor recognized his talent with a scalpel. A prolific researcher as well as a sought-after surgeon, he has published extensively in peer-reviewed scientific journals. In 2012, while at the University of Maryland, he performed what was then the most ambitious face transplant ever, on a man who’d lost his lips, nose, and jaws in a shotgun accident; tissue from the hairline to the neck was replaced, including both jawbones and part of the tongue.
That surgery led to the recruitment of Dr. Rodriguez the following year by NYU Langone, which sought to build a face transplant program of its own and expand its existing transplant program. “There’s a tremendous amount to learn from face transplants,” says Robert I. Grossman, MD, the Saul J. Farber Dean and CEO of NYU Langone. “How do we advance our microsurgical techniques? How do we improve interdisciplinary teamwork in the operating room? What are the psychiatric consequences? The surgery is a tour de force.”
So much so that it required assembling a team of over 100 physicians, nurses, technicians, and support staff, drawn from multiple disciplines, including plastic surgery, anesthesiology, radiology, ophthalmology, critical care, physical medicine and rehabilitation, psychology, psychiatry, and social work. It also required finding an inaugural patient. The ideal candidate would be someone capable of handling the emotional stresses surrounding the procedure, of understanding the potential pitfalls, and of following the regimen necessary for a successful long-term outcome—not only taking an array of medications, but avoiding activities that could compromise the health of the graft, such as cigarette smoking or excessive sun exposure.
Hardison, who had approached Dr. Rodriguez before the surgeon’s move to New York, was already in the running, but before he could be selected, he had to undergo a battery of physical, psychological, and other evaluations. Dr. Rodriguez traveled to Senatobia (pop. 8,165) with several team members—administrator Bernstein; plastic surgeon Alexes Hazel, MD; psychologist Aileen Blitz, PhD; and senior social worker Sally Klein—to assess Hardison’s social and physical environment. They met with his friends, family members, primary care physician, pharmacist, and pastor. In the end, Hardison prevailed over two other candidates. “Patrick had proven his resilience over many years and many surgeries,” Dr. Blitz explains. “Although he was divorced, he was very involved with his kids and his community. He had lots of people behind him, including his old firefighting buddies and a brother who was willing to sign on as his designated caregiver. He was bright and motivated. All his ducks were in a row.”
And he fully grasped the possibility of failure. “There are things in life that are worse than dying,” Hardison said, whenever the topic came up. “I’ve known that for 14 years.”
He was placed on the transplant list in August 2014, and the team began rehearsing for his surgery. There were numerous dry runs, using paired cadavers. Team members drew up patient flow charts and organized surgical instruments into dozens of trays. Other members crafted a business plan in which a grant from NYU Langone would cover the first 90 days of medical costs, and Mississippi Worker’s Comp would then take over.
Hardison, meanwhile, journeyed northward for monthly consultations. His health and medications were closely monitored. He received psychological and pain-management counseling (including instruction in techniques such as self-hypnosis and mindfulness training, aimed at reducing his need for prescription analgesics). Then he flew back home and waited.
The transplant team waited, too, perpetually on call. “If anyone wanted to travel, they’d let me know first,” Bernstein recalls. “I’d say, ‘You can go, but where can I reach you? And if we need you, how will you get back?’”
Because face transplants are so rare, would-be recipients don’t have to line up for an organ. But a shortage of donors plagues every area of transplant medicine, and a patient seeking a new face draws from a particularly narrow pool. Besides the usual requirements of tissue matching, the graft must be appropriate in appearance. For Hardison, that ideally meant finding a fair-skinned male donor—no easy task in New York City, whose population is just 33 percent non-Hispanic white. A further obstacle was a New York State regulation barring the transport of a dead or brain-dead body across more than one county line.
Although NYU Langone representatives eventually persuaded state officials to alter the rule, the change made little difference. By the one-year anniversary of Hardison’s search, only two potential donors had appeared—one whose complexion was a good match but whose tissue profile wasn’t, and another a darker complexion. Hardison was willing to accept the second candidate, but the man’s family withdrew him from consideration.
By midsummer 2015, Hardison was nearing despair. Then, on August 12, LiveOnNY—the nonprofit that coordinates organ donations in the New York metropolitan area—notified Dr. Rodriguez that another face had become available. It belonged to David Rodebaugh, a 26-year-old bike mechanic who’d sustained a massive head injury in a cycling accident and was now brain dead. Rodebaugh was tall and fair, like Hardison, and according to his grieving mother, he’d always dreamed of becoming a firefighter. Instead, his own tragedy had given him the chance to relieve a former firefighter’s suffering.
The next morning, when the initial lab work came back looking promising, Dr. Rodriguez asked Hardison to get on a plane to New York. By the time it landed, the results were in: Rodebaugh was an excellent cross-match. Dr. Rodriguez and Bernstein took out their phone trees and summoned the team. Rodebaugh’s body was transported from a hospital in Brooklyn to NYU Langone, where technicians took CT scans and began prepping him for surgery. That evening, Hardison checked in, accompanied by his older sister and a close friend.
At 7:00AM on August 14, Dr. Rodriguez and three surgical assistants began the dissection of Rodebaugh’s face, meticulously identifying and preserving nerves and blood vessels. Meanwhile, surgeons allocated by LiveOnNY prepared to harvest Rodebaugh’s heart, kidneys, and liver for transplant in four other patients. Soon afterward, Hardison arrived in the adjoining OR. As IV lines delivered anesthesia and immunosuppressants, the surgical team set to work removing his mask of scar tissue. Around 11:00AM, 3-D–printed cutting guides based on CT scans of Rodebaugh’s head arrived from Colorado (see “Making the Cut”). In the donor room, Dr. Rodriguez began sawing portions of bone from Rodebaugh’s facial skeleton (the chin, nasal structure, and a sliver of the cheekbones), leaving them attached to the inner skin. This technique, which had never been used before, would help ensure that the face was properly secured to fit its new owner.
Shortly before 7:00PM, the surgeon went next door to finish the tailoring of Hardison’s facial skeleton. Then, he returned to the donor room and completed the operation on Rodebaugh. Dr. Rodriguez placed the donor’s face in a basin of preservative solution and wheeled it to the recipient room on a rolling stand. He draped the hood of flesh over Hardison’s head, snapped the bones into place, and secured them with plates and screws. Peering through a microscope, he stitched the major sensory nerves together—others were expected to grow back over time—and began connecting the major blood vessels.
Hardison’s internal jugular vein was larger than Rodebaugh’s, and a suture failed; the patient quickly lost two pints of blood. Dr. Rodriguez stopped the flow by clamping the external carotid artery. After creating a new junction, he loosened the clamp, and the face turned a reassuring pink. It also began to swell, as expected, ballooning to 50 percent larger than its normal size.
The team continued to work through the night, redraping the eyelids and joining nostrils and outer lips to their respective mucosa. At 9:30AM, on August 15, more than 26 hours after making his initial incision, Dr. Rodriguez finished sewing up the scalp. “Congratulations, everyone,” he said, and there were hugs and high-fives all around.
“After the surgery is when the real work begins,” says Nicole Sweeney, NP, who coordinates patient care for the Face Transplant Program. During the first week, there were late-night scares involving fluctuations in blood pressure and an unstable airway. Hardison needed therapy to relearn how to speak and swallow; he had bouts of frustration and anxiety. On day nine, when Dr. Rodriguez handed him a mirror for the first time, his face was still so swollen that his mouth wouldn’t close. He gazed silently at the reflection, his expression impossible to read.
But Hardison was able to blink for the first time since 2001, and his progress in other areas proved rapid. By early October, he was holding conversations and eating solid food. When his kids came for their first visit, tears were shed, but then the whole gang went out for barbecue. Two weeks later, Hardison was discharged to outpatient status; he moved to an apartment across the street from the hospital, returning daily for ongoing rehabilitation. He took a shopping trip to Macy’s and was overjoyed when no one stared.
In November, he returned to Senatobia, where a parade was held in his honor. Hardison rode in an open limousine and was serenaded by honking fire trucks. He enjoyed a Thanksgiving feast with his family. He appeared on Nightline, where he spoke passionately of his gratitude to Rodebaugh and his loved ones. He showed the first inklings of a smile.
That didn’t mean he was out of the woods. Although no face transplant patient has died during surgery, three have perished within the first year, either from infections or complications related to rejection. Indeed, almost every patient has had an episode of acute rejection within the first 90 days. But by February, when this article went to press, Hardison had not. Bruce Gelb, MD, assistant professor of surgery, and director of renal transplantation at NYU Langone, who designed his immunosuppressant regimen, credits a postoperative dose of rituximab, a monoclonalantibody used to treat blood cancers and autoimmune disorders that has also shown efficacy in preventing rejection in kidney transplants. Hardison is the first face-transplant patient to receive rituximab (in addition to the standard combination of thymoglobulin, tacrolimus, and low-dose prednisone, and his continued health may encourage the use of this medication for those who follow.
Dr. Rodriguez was recently awarded $2.5 million by the Defense Department to aid in continued face-transplant research. He’s already looking for his next patient. But Hardison will remain in his care for years to come, returning for regular checkups as well as occasional surgeries to adjust his new features, and consulting as needed with the rest of the team. “This is not an operation for everyone,” Dr. Rodriguez says. “It’s for very courageous people. We’re in awe of Patrick, and we’ll be here for him as long as he needs us.”




