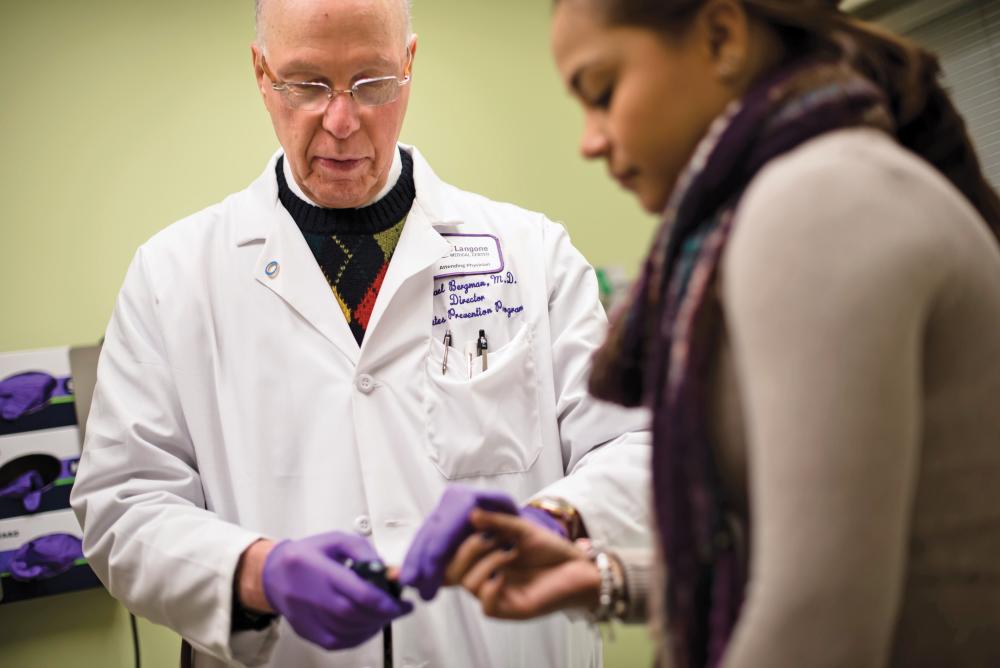
Photo: Karsten Moran
A century ago, Elliott Joslin, MD, one of the first physicians in the US to specialize in diabetes, noted that “real headway against the ravages of this disease begins with prevention rather than treatment.” Few people understand that better than endocrinologist Michael Bergman, MD, director of the new Diabetes Prevention Program at NYU Langone. Dr. Bergman has been treating and studying the disease for 35 years, has edited a comprehensive textbook on global diabetes prevention, and has spent several years searching for a biological marker to identify those at early risk for developing diabetes.
Last year, Dr. Bergman was tapped to head the new program, overseeing a team of endocrinologists, nutritionists, and diabetes educators. NYU Langone was nationally ranked in diabetes and endocrinology on U.S. News & World Report’s Best Hospitals 2015–16 Honor Roll.
In the US, an estimated 29 million adults have type-2 diabetes, in which the body doesn’t make enough insulin to process sugar properly or can’t use insulin because cells have become desensitized to it. An estimated 1.25 million children and adults have type-1 diabetes, in which the body does not make insulin due to the destruction of insulin-producing cells in the pancreas. The precursor to diabetes is called prediabetes—blood sugar levels are higher than normal but not high enough to be classified as diabetes. The Diabetes Prevention Program targets people in this group, which numbers an estimated 86 million adults (one in three), for early intervention. Diabetes and prediabetes are both diagnosed through blood tests.
Dr. Bergman stresses that the “pre” doesn’t mean that the condition is benign. “I consider prediabetes a disease in its own right,” he says, “because it can result in similar complications—heart disease, stroke, and other associated disorders—but on a much smaller scale.” Without intervention, he adds, up to 30 percent of those with prediabetes will develop diabetes within five years, and up to 70 percent will do so eventually.
Only 10 percent of those with prediabetes are diagnosed, and fewer still receive clear guidance about where to go and what to do to get help. The reasons, Dr. Bergman explains, are partly because the condition typically poses no symptoms and partly because many physicians are not on the lookout for it.
“Every time I see someone get the diagnosis of diabetes,” says Dr. Bergman, “I say to myself, ‘Did this have to happen?’ Prediabetes is a wake-up call. I see primary care physicians as the sweet spot because they can identify the problem early. The progression to full-blown diabetes can take a decade or even longer. That’s a big window of opportunity for prevention.”
Dr. Bergman and his team support patients through challenging lifestyle changes and self-management by creating a flexible, personalized plan of action and expert counseling. The emphasis is on eating carefully, maintaining a healthy weight, exercising regularly, managing stress, and getting adequate sleep. The screening process often begins with a simple questionnaire (see Prediabetes Screening Test) that may signal the need for a blood test to confirm a mounting blood sugar problem, followed by more specialized tests.
“Every time I see someone get the diagnosis of diabetes, I say to myself, ‘Did this have to happen?’”
“With our aging, increasingly overweight population,” notes Steven Hodak, MD, associate director of the Division of Endocrinology, Diabetes, and Metabolism, “this is a critical time to identify people at risk and offer them relatively simple interventions that can avoid serious medical problems down the road.”
Studies show that in most cases, diabetes can be delayed or even prevented with lifestyle modifications. “If you’re overweight, you can reduce your risk by 58 percent by losing 5 to 7 percent of your body weight and exercising moderately for a total of 150 minutes a week,” Dr. Bergman explains to patients to empower them. “That’s considerably more effective than medication.”