Thomas Graves thought he had no chance of replacing his faulty aortic valve without surgery—until he came to NYU Langone.

Thomas Graves was back to racing sailboats just a week after his transcatheter aortic valve replacement (TAVR) procedure.
Photo: Brad Trent
When Thomas Graves, a 73-year-old from Bridgeport, Connecticut, retired as a marketing executive 10 years ago, he had no intention of taking it easy. He kept up his fitness regime, working out 3 times a week, and raced his 37-foot sailboat, Bad Dog, with the Cedar Point Yacht Club every Wednesday.
But about two years ago, activities he once did almost effortlessly, like walking up hills with his dog or training on the elliptical machine, began to leave him winded. A local cardiologist recommended a stress test. “It was a struggle to complete it,” says Graves.
His diagnosis was sobering: Graves had aortic stenosis, a narrowing of the aortic valve opening, which restricts blood flow from the left ventricle to the body’s main artery. The progressive disease affects an estimated 1.5 million Americans, and in Graves’ case it left him at long-term risk for heart failure. Since he was otherwise healthy, the doctor recommended open heart surgery to insert a replacement valve.
“I didn’t want my chest cracked open,” says Graves, “but nobody else was offering me an alternative.”
So Graves sought out a better option, and he ultimately found it at the Heart Valve Center at NYU Langone Health. The center’s surgeons have been at the forefront of many pioneering treatments for valve disease. Among these is a nonsurgical technique called transcatheter aortic valve replacement, or TAVR, widely used as an alternative for patients considered too frail to endure the rigors of open heart surgery and the months-long recovery.
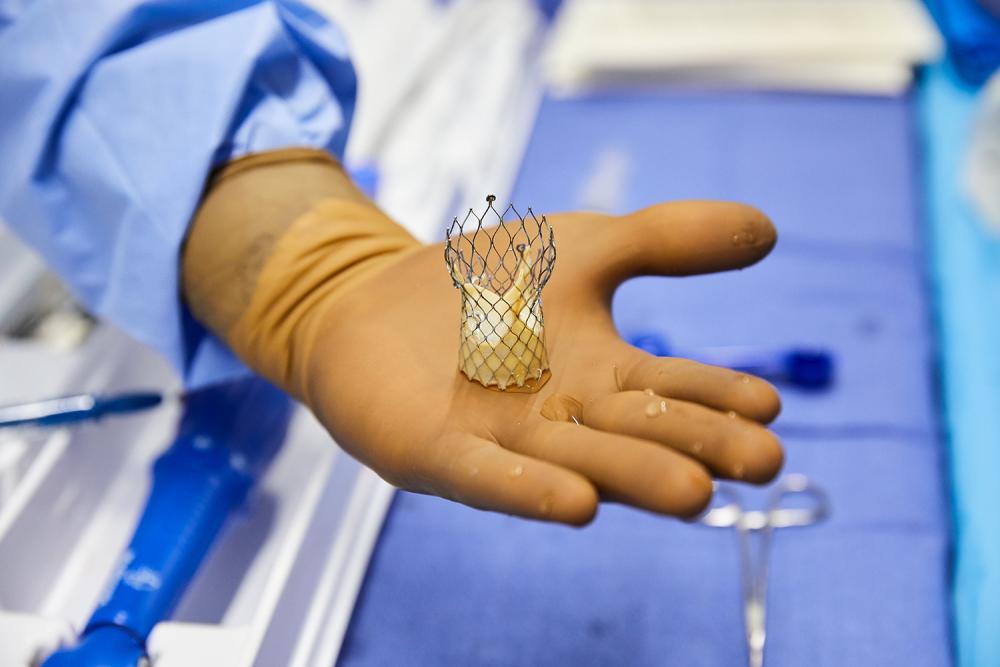
Using live imaging as a guide, surgeons thread an artificial valve made of animal tissue and a metal mesh stent through a tiny puncture in the groin, up through the femoral artery, and into the heart. There, the device is deployed inside the old valve and expanded to restore normal blood flow.
Mathew R. Williams, MD, director of the Heart Valve Center and chief of the Division of Adult Cardiac Surgery, has performed over 3,000 TAVR procedures, more than any other U.S. surgeon. The majority have been completed on high-risk patients. Yet this demographic is quickly changing. Last year, Dr. Williams coauthored a study published in the New England Journal of Medicine showing that the technique is an equivalent or superior alternative for patients who are deemed healthy enough for open heart surgery.
“The treatment of heart valve disease has progressed rapidly during the past five years,” says Dr. Williams, who is the first person in the U.S. to be dual-trained in interventional cardiology, which relies heavily on catheter-based procedures, and cardiac surgery, which involves open surgery. “Replacing valves through catheterization has been like going from a model T to a Tesla.”
The center is currently leading or participating in more than a dozen clinical trials to assess new catheter-based treatments, indications, and devices. Graves was accepted into one such trial last year. It was randomized, meaning he had a 50-50 chance of getting open heart surgery, so, in his words, “When they told me I was selected for TAVR, I felt like I’d won the lottery.”
In a sense, he did. Instead of a 4- to 6-hour operation that requires stopping the heart and using a heart–lung bypass machine, Graves got a new valve in about 45 minutes. He was given local anesthesia, needed not a single stitch, and walked out of the hospital the next day, as many patients undergoing TAVR do.
“Dr. Williams is supremely confident in his ability,” says Graves. “You can’t ask for more from a surgeon who is about to work on your heart.”
Experience with this state-of-the-art technique counts for a lot. Maneuvering the pencil-wide catheter through the artery and precisely positioning the artificial valve into place demands an elite team of experts, including Muhamed Saric, MD, PhD, director of echocardiography and clinical director of noninvasive cardiology, and Cezar S. Staniloae, MD, an interventional cardiologist. Thanks to their experience, the risk of stroke for patients undergoing TAVR at the NYU Langone Heart Valve Center is six times lower than the national average.
While data are still emerging on the long-term benefits of the artificial valves, Dr. Williams believes “TAVR will eventually become the standard method for an overwhelming majority of patients with aortic stenosis,” he says.
A week after the procedure, Graves was back to his normal activities—including skippering a crew of five on the Long Island Sound and working out. “If you need an aortic valve replacement and have the option of TAVR,” he says, “I would recommend NYU Langone in a heartbeat.”