Breast Cancer Screening
At NYU Langone’s Perlmutter Cancer Center, the goal of breast cancer screening is to identify cancer early, when it can be most effectively treated. The important benefit of early detection is that it can lead to the most effective treatment.
Early detection may also mean that you require less extensive treatment and experience fewer side effects.
Our doctors follow the current recommendations of the American Cancer Society, which direct women to become familiar with how their breasts look and feel and to report any changes, such as the appearance of a lump, to their doctors as soon as possible.
They also advise having a mammogram—the X-ray test that’s considered the gold standard for breast cancer screening—every year starting at age 40, with the option to start screening between the ages of 40 and 44. Women age 55 and older may choose to have a mammogram every other year or continue with annual screening. Mammograms are the primary test used to screen for breast cancer, but they may not be the only one our doctors recommend.
Our doctors advise women to have a mammogram every year starting at age 40.
Our doctors can recommend a more personalized screening plan based on your individual risk of developing breast cancer, taking into account factors such as family history and whether you have a genetic mutation associated with breast cancer. If your doctor determines you are at increased risk, they may recommend having additional screening tests starting before age 40.
We offer a full range of imaging tests at several locations, including Perlmutter Cancer Center, the Joan H. Tisch Center for Women’s Health, and the Laura Perlmutter Center for Women’s Imaging.
Screening Tests
Our fellowship-trained breast imaging radiologists interpret the images and provide a full report of your mammogram and breast ultrasound exam. Most reports are available to patients within 6 to 10 business days. You can view the results through your NYU Langone Health MyChart account on your computer, or by using the NYU Langone Health app on a mobile device.
The results are also provided directly to your referring physician, whom you may contact to discuss further.
Mammogram
During a mammogram, your breasts are gently compressed between two plates that are attached to a mammography unit, an X-ray machine designed specifically for mammograms. The unit flattens breast tissue, making any tumors easier to see. The technician takes multiple two-dimensional images of the breasts.
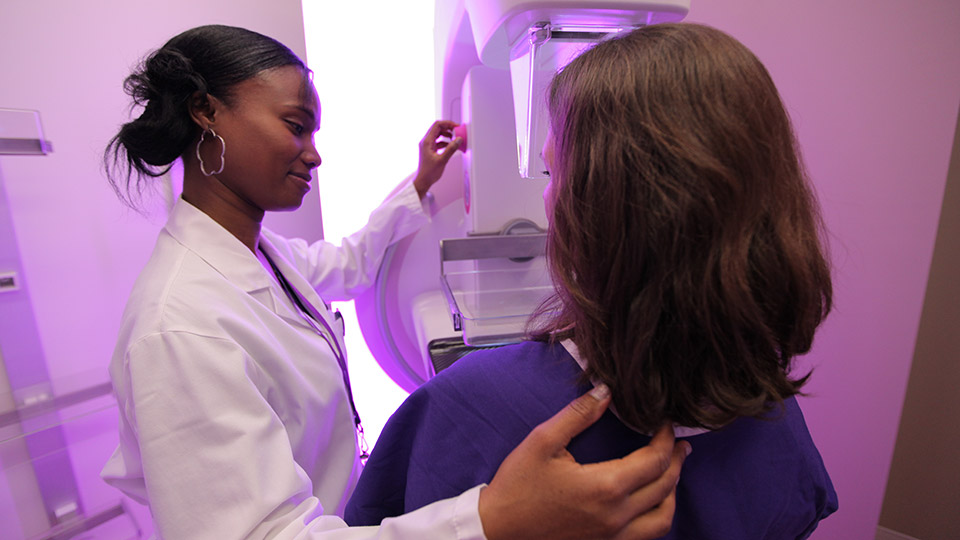
At Perlmutter Cancer Center, mammographic images are digitized and stored on a computer. This enables doctors to enhance and magnify the images while reviewing them. They look for suspicious growths or calcium deposits, which can be a sign of cancer.
Three-Dimensional Mammogram
During a three-dimensional mammogram, known as breast tomosynthesis, X-ray images are taken from multiple angles to create three-dimensional pictures of the breast.
The benefits of breast tomosynthesis are currently being investigated. This approach may help doctors detect any suspicious growths, especially in women who have “dense” breasts, which contain more fibrous and glandular tissue than fatty tissue. While this is normal, it can make breast cancer difficult to detect on traditional mammograms.
Breast Ultrasound
In ultrasound, sound waves create images of the breasts. Ultrasound can help determine if a breast mass is solid or filled with liquid (cystic). This test is often used in combination with a mammogram in women who have dense breast tissue.
Breast MRI
In an MRI, a magnetic field and radio waves are used to produce computerized, three-dimensional images of the breasts. Our doctors may recommend a breast MRI if mammogram images are unclear or if you are at high risk of developing breast cancer.
High Risk Screening Program
We offer a screening and prevention program for women at high risk of developing breast cancer. Our team of medical oncologists, surgical oncologists, and staff members works with you to help you gain a clear understanding of your breast cancer risk factors, how your risk of developing the condition evolves as your life changes, and what you can do to manage your risk.
Our screening and prevention program is tailored to healthy women who are at high risk of developing breast cancer.
Through this program, each woman receives a thorough physical examination, a review of her medical history by an oncologist, and routine and advanced screening examinations that may consist of clinical breast exams, mammograms, ultrasounds, and MRIs.
The program also includes surveillance for associated cancer risk, including ovarian, colon, uterine, pancreatic and other stomach cancers, thyroid cancers, and melanoma.
Women who are found to be at high risk for breast cancer receive individualized preventive care to help minimize and manage their risk. This may include nutritional, psychological, and genetic counseling, preventive treatments—for example, tamoxifen or access to clinical trials that evaluate various approaches to cancer prevention—and risk-reducing surgery.
Perlmutter Cancer Center researchers collect information about the health of high-risk women in a longitudinal registry, meaning medical information is repeatedly evaluated over a long period of time to help investigators discover which screening and preventive measures are most effective.
Non-Modifiable Risk Factors
Women are considered to be at high risk for breast cancer if they have a family history of the disease or genetic mutations. The most common cause of hereditary breast cancer are abnormal versions of the BRCA1 or BRCA2 genes, which are also called the “breast cancer genes.”
Normal versions of the BRCA1 and BRCA2 genes produce proteins that help prevent cancer growth. Abnormal, or mutated, versions of these genes raise the risk that breast cancer may develop.
These genetic mutations are rare in the general population; they occur more often in people of Ashkenazi Jewish descent. BRCA1 and BRCA2 testing, which usually involves a blood test, is available at NYU Langone. Abnormal versions of other genes, such as PALB2, CHEK2, and PTEN, may also increase the risk of inherited breast cancers. These genetic changes are less common and are not as high risk as BRCA mutations.
Genetic mutations linked to cancers of the colon, uterus, and thyroid, as well as melanoma, may also increase the risk of breast cancer. Doctors at NYU Langone can also test for and identify these genetic mutations. Women with high-risk mutations can choose to have prophylactic mastectomy before any cancer develops through our breast in a day surgery.
Our genetic counseling and testing services can help women with these mutations better understand their risk of developing cancer. Our counselors can recommend support services that help you manage the psychological effects of testing positive for these mutations.
In addition to your family history and the results of genetic testing, doctors take other risk factors into account when developing a breast cancer screening plan for you. Certain conditions can increase your risk of developing cancer, including lobular carcinoma in situ and atypical hyperplasia, an overgrowth of cells in the milk ducts or milk-producing glands.
Prior radiation therapy—the use of high energy beams to destroy cancer cells—for conditions such as Hodgkin lymphoma and thyroid cancer can also increase your risk of breast cancer.
Some lifestyle factors may increase your risk of developing breast cancer. For example, studies show that smoking and other forms of tobacco consumption may raise the risk. Our doctors strongly urge people to quit smoking. Our specialists offer an effective Tobacco Cessation Program to help you stop for good.
Tobacco Cessation Program
Smoking can increase your risk of developing breast cancer. We can help you quit.
Learn MoreDrinking alcohol may also increase the risk of breast cancer. Additionally, having excess weight, meaning having a body mass index (BMI) of 25 to 29.9, or obesity, meaning a BMI of 30 or higher, has also been linked to breast cancer.
Using combination hormone therapy after menopause—which includes estrogen and progesterone—can also raise breast cancer risk. These hormones may fuel breast cancer growth.
One of the strongest risk factors for developing breast cancer is age. A woman’s risk increases as she gets older.
Meet Our Doctors
Perlmutter Cancer Center specialists provide care and support during treatment.
Browse Doctors